What Is Inflammation? A Complete Guide to Better Health
Inflammation is a natural process. It helps your body fight infections and heal injuries. It also protects you from harm. In fact, it plays an important role in your immune system. However, when it lasts a long time, it can harm your body. As a result, it may lead to serious health problems. Therefore, understanding inflammation is important for long-term health.
🧠 What Is Inflammation?
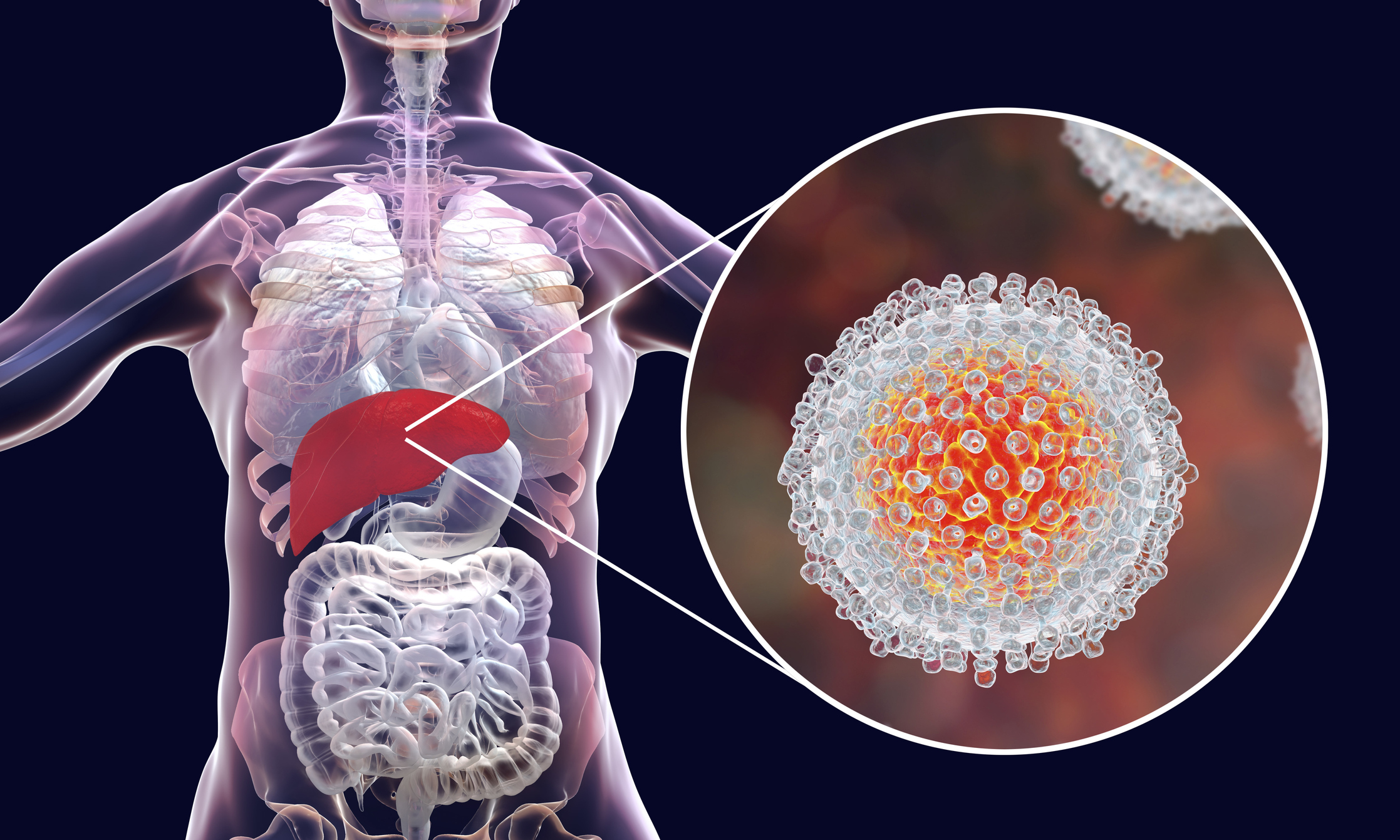
This condition is your body’s response to injury, infection, or harmful substances. In simple terms, it shows that something is wrong. Therefore, it helps protect your body.

There are two main types:
1. Acute Inflammation
This type is short-term and helpful. For example, when you cut your finger, you may see redness and swelling. These are signs of healing. As a result, this type supports recovery.
2. Chronic Inflammation
This type is long-term and harmful. In contrast, it does not help with healing. Over time, it can damage tissues and organs. It may continue even without injury. Consequently, it can lead to serious health problems.
⚠️ Signs and Symptoms of Inflammation
If inflammation occurs, your body may show some signs. For example, you may notice:
- Redness and swelling
- Pain or tenderness
- Heat in the affected area
- Fatigue
- Joint stiffness
However, chronic inflammation may not show clear signs. As a result, it can be hard to detect early.
🚨 Causes of Inflammation
Several factors can trigger inflammation. Some of the most common include:
1. Poor Diet
Diets high in sugar, processed foods, and unhealthy fats can increase inflammation. As a result, your body may remain in a constant inflammatory state.
2. Lack of Physical Activity
A sedentary lifestyle slows down body functions. Consequently, it may contribute to chronic inflammation.
3. Chronic Stress
Stress increases cortisol levels. Over time, this can disrupt your immune system and promote inflammation.
4. Smoking and Alcohol
These habits introduce harmful substances into the body. In addition, they weaken your natural defense system.
5. Obesity
Excess body fat produces inflammatory chemicals. Therefore, maintaining a healthy weight is important.
It can affect many parts of the body. It may occur in the joints, skin, or gut. For example, you may feel pain, swelling, or warmth in one area. Sometimes, you may feel tired or weak. In addition, long-term chronic conditions can make daily life harder. It may slow down healing and reduce energy levels.
However, small changes can help control it. Eating fresh food, moving your body, and sleeping well can improve your health. Also, drinking enough water helps your body work better. So, simple habits can lower immune response and help you feel better each day.
Your daily habits play a big role in inflammation. For example, eating too much junk food can raise it. Foods high in sugar and fat can harm your body. On the other hand, fresh fruits and vegetables can help reduce it. They give your body the nutrients it needs. In addition, regular movement is important. You do not need heavy exercise. A short walk each day can help. It keeps your body active and improves blood flow.
🧬 Why Chronic Inflammation Is Dangerous
Chronic inflammation is linked to many serious conditions. For example, it is associated with:
- Heart disease
- Type 2 diabetes
- Arthritis
- Certain cancers
In addition, it can damage healthy cells and speed up aging. As a result, your health may get worse over time. Therefore, managing this process is important.
It can affect many parts of the body. It may occur in the joints, skin, or gut. For example, you may feel pain, swelling, or warmth in one area. Sometimes, you may feel tired or weak. In addition, long-term chronic conditions can make daily life harder. It may slow down healing and reduce energy levels.
However, small changes can help control it. Eating fresh food, moving your body, and sleeping well can improve your health. Also, drinking enough water helps your body work better. So, simple habits can lower immune response and help you feel better each day.
Your daily habits play a big role in inflammation. For example, eating too much junk food can raise it. Foods high in sugar and fat can harm your body. On the other hand, fresh fruits and vegetables can help reduce it. They give your body the nutrients it needs. In addition, regular movement is important. You do not need heavy exercise. A short walk each day can help. It keeps your body active and improves blood flow.
🥗 How to Reduce Inflammation Naturally
The good news is that you can control inflammation with simple habits.
1. Eat an Anti-Inflammatory Diet
Eat fruits, vegetables, nuts, and healthy fats. In particular, antioxidant-rich foods help fight inflammation.
2. Exercise Regularly
Physical activity improves blood flow. As a result, it helps lower inflammation.
3. Get Enough Sleep
Sleep helps your body recover. Therefore, aim for 7–8 hours each night.
4. Manage Stress
Practice yoga, meditation, or deep breathing. As a result, stress levels drop and inflammation reduces.
5. Stay Hydrated
Drink enough water daily. In addition, it helps remove toxins and supports your body.
Inflammation is a natural process. It helps your body fight infections. It also helps heal injuries. In addition, it protects you from harm. In fact, it is an important part of your immune system. However, when it lasts too long, it can harm your body. It may damage tissues over time. As a result, it can lead to serious health problems. Therefore, it is important to understand it. This helps you stay healthy in the long term.
💡 The Truth About Inflammation
Many people think all inflammation is harmful. However, this is not true. In fact, short-term inflammation helps your body heal. On the other hand, long-term inflammation is the real problem. Therefore, the goal is to control it, not remove it completely.
✅ Conclusion
In conclusion, inflammation is a key part of your body’s defense. However, when it lasts too long, it can harm your health. Fortunately, simple habits can help reduce it. For example, a healthy diet, exercise, and stress control make a big difference. Ultimately, balance is the key to long-term health.
📚 References
- World Health Organization (WHO) – Chronic Diseases and Inflammation
- Harvard Health Publishing – Understanding Inflammation and Its Effects
- Mayo Clinic – Inflammation: Causes and Treatment
- National Institutes of Health (NIH) – Inflammation and Immune Response
Medications that have been suggested by doctors worldwide are available on the link below
https://mygenericpharmacy.com/category/disease/inflammation