Diabetes Symptoms, Causes, Types & Management | Complete Guide
Learn about diabetes, including its causes, symptoms, different types, and effective management strategies. Discover lifestyle tips, treatment options, and prevention methods to maintain healthy blood sugar levels.

Diabetes mellitus is one of the most common chronic conditions worldwide, affecting millions of people across all age groups. In the WHO European Region alone, at least 64 million adults and around 300,000 children and adolescents are estimated to be living with diabetes. This condition occurs when your body cannot maintain healthy blood glucose (sugar) levels, leading to serious health complications if left untreated or poorly managed.
The good news is that with proper understanding, early diagnosis, and consistent management, people with diabetes can live long, healthy, fulfilling lives. This comprehensive guide will walk you through everything you need to know about diabetes—from its causes and types to symptoms, diagnosis, and proven management strategies.
What Is Diabetes?
Diabetes is a chronic disease that occurs either when the pancreas does not produce enough insulin or when the body cannot effectively use the insulin it produces. Insulin is a hormone that regulates blood glucose and allows glucose to enter cells for energy.
Glucose comes from two main sources: food and the liver. During digestion, sugar is absorbed into the bloodstream, where it normally enters cells with the help of insulin. The liver also stores and makes glucose. When glucose levels are low, such as when you haven’t eaten in a while, the liver breaks down stored glycogen into glucose to keep your glucose level within a typical range.
In diabetes, this system breaks down. Sugar builds up in the bloodstream because the pancreas doesn’t produce enough insulin, the insulin doesn’t work properly, or both.
Types of Diabetes: Understanding the Differences
Diabetes is not a single disease but a group of conditions with different causes and characteristics. Proper classification is crucial for informing personalized therapy.
Type 1 Diabetes
Type 1 diabetes is an autoimmune condition where the body’s immune system attacks and destroys the insulin-producing cells in the pancreas. This means the body cannot make any insulin at all.
Key characteristics:
- Accounts for approximately 5-10% of all diabetes cases
- Often diagnosed in childhood or young adulthood, but it can develop at any age
- Symptoms tend to appear quickly
- Requires daily insulin treatment through injections or a pump
- Cannot currently be prevented
- People with type 1 diabetes are at increased risk for other autoimmune disorders, such as Hashimoto’s thyroiditis, Graves’ disease, and coeliac disease
There are three distinct stages of type 1 diabetes:
- Stage 1: Autoimmunity in the absence of hyperglycaemia or symptoms
- Stage 2: Autoimmunity with dysglycaemia but without symptoms
- Stage 3: Autoimmunity with hyperglycaemia and symptoms
Type 2 Diabetes
Type 2 diabetes is characterized by ineffective use of insulin. The body either doesn’t make enough insulin or the insulin it makes doesn’t work properly—a condition known as insulin resistance.
Key characteristics:
- Accounts for 90-95% of all diabetes cases
- Often develops in middle age, although prevalence is rising among children and adolescents
- Symptoms can be mild and develop slowly; diagnosis can often be delayed until after complications have already occurred
- Risk factors include excess weight (especially around the waist), low levels of physical activity, family history, and certain ethnic backgrounds
- Can sometimes be treated without medication through lifestyle changes
- Can be prevented or delayed through healthy lifestyle choices
Gestational Diabetes
Gestational diabetes is characterized by high blood sugar levels during pregnancy. It typically develops in the second or third trimester in women who did not have diabetes before pregnancy.
Key points:
- Usually resolves after the baby is born
- Increases the mother’s risk of developing type 2 diabetes later in life
- Requires careful management to protect both mother and baby
- Babies born to mothers with gestational diabetes have a higher risk of developing obesity and type 2 diabetes later in life.
Prediabetes
Prediabetes refers to elevated glucose or glycated hemoglobin (HbA1C) levels that do not meet the criteria for diabetes but indicate abnormal carbohydrate metabolism. It’s an intermediate state between normoglycaemia and diabetes.
Key facts:
- Significantly increases the risk of progressing to diabetes and developing cardiovascular disease
- Can be identified by:
- Impaired fasting glucose (FPG of 100-125 mg/dL)
- Impaired glucose tolerance (2-hour PG during OGTT of 140-199 mg/dL)
- HbA1C levels between 5.7% and 6.4%
- This risk can be drastically reduced through intensive lifestyle interventions
Recognizing Diabetes Symptoms
Diabetes symptoms depend on how high your blood sugar is. Some people, especially those with prediabetes, gestational diabetes, or early type 2 diabetes, may not have symptoms at all. In type 1 diabetes, symptoms tend to come on quickly and be more severe.
Important Distinctions
Type 1 diabetes: Symptoms often appear quickly, and delayed diagnosis and treatment can lead to diabetic ketoacidosis (DKA), a life-threatening condition.
Type 2 diabetes: Symptoms can be easier to miss because they develop more slowly, especially in the early stages. Some people may have diabetes for up to 10 years without knowing it.
When to see a doctor: If you or your child experience any possible diabetes symptoms, contact your health care provider. The earlier the condition is diagnosed, the sooner treatment can begin.
Risk Factors: Who Is at Risk?
Risk factors differ depending on the type of diabetes.
Type 1 Diabetes Risk Factors
- Family history (genetic predisposition)
- Age (more common in those under 40, but can occur at any age)
- Certain genetic markers
- Geography (rates vary by country)
Type 2 Diabetes Risk Factors
Type 2 diabetes has numerous risk factors :
Lifestyle factors:
- Being overweight or obese, especially with excess weight around the waist
- Low level of physical activity
- Poor diet
- Smoking
Non-modifiable factors:
- Increasing age (risk increases after 40; over 25 for certain ethnic groups)
- Family history of diabetes
- Ethnicity (higher risk in people of South Asian, African, African-Caribbean, Chinese, Hispanic, American Indian, and Asian American descent)
- History of gestational diabetes
- Polycystic ovarian syndrome (PCOS)
- High blood pressure or high cholesterol
Gestational Diabetes Risk Factors
- Being overweight or obese
- Previous history of gestational diabetes
- Family history of diabetes
- Being over age 25
- Certain ethnic backgrounds
Diagnosis: Tests and Screening
Diabetes can be diagnosed through relatively inexpensive testing of blood glucose. However, an estimated 1 in 3 people in some regions remains undiagnosed.
Screening Guidelines
The American Diabetes Association (ADA) recommends screening for :
- Anyone with a body mass index higher than 25 (23 for Asian Americans) who has additional risk factors (high blood pressure, inactive lifestyle, family history, etc.)
- Anyone older than age 35 (initial screening, then every three years if normal)
- Women who have had gestational diabetes (every three years)
- Anyone diagnosed with prediabetes (every year)
- Anyone with HIV
Treatment: Managing Diabetes Effectively
Treatment approaches differ based on the type of diabetes but share the common goals of controlling blood glucose levels, preventing complications, and optimizing quality of life.
Type 1 Diabetes Treatment
Type 1 diabetes must be managed with insulin. This involves:
- Daily insulin injections or continuous infusion through a pump
- Carbohydrate counting to balance food with insulin doses
- Regular blood glucose monitoring
- Healthy eating and regular physical activity
The ADA recommends using insulin analogues or inhaled insulin rather than injectable human insulins for better outcomes.
Type 2 Diabetes Treatment
Type 2 diabetes can be treated through a combination of approaches :
Lifestyle modifications (foundation of treatment):
- Healthy eating: Choose foods lower in fat and calories and higher in fiber. Focus on fruits, vegetables, and whole grains.
- Physical activity: Aim for at least 150 minutes of moderate aerobic activity per week (about 30 minutes, 5 days a week)
- Weight management: Losing even 5-10% of body weight can significantly improve blood sugar control. In some cases, weight loss can lead to diabetes remission (well-controlled blood glucose for at least 3 months without needing medicines).
Medications:
- Oral medications (such as metformin, which is often the first-line treatment)
- Non-insulin injectable medications
- Insulin therapy (some people with type 2 diabetes may eventually need insulin)
The ADA recommends starting treatment with combination therapy to quickly reach individualized treatment goals, rather than a more traditional stepwise intensification of therapy.
Gestational Diabetes Management
- Blood glucose monitoring
- Healthy eating plan
- Physical activity
- Insulin if needed
- Monitoring of the baby’s growth
Prediabetes Management
For individuals at high risk of developing type 2 diabetes, intensive lifestyle modifications should be initiated :
- Weight reduction of at least 7% through healthy calorie-controlled eating plans
- ≥150 minutes per week of moderate-intensity physical activity
- Sleep optimization (aim for approximately 7 hours daily)
- Mediterranean or DASH dietary patterns
- Consider metformin for those at very high risk
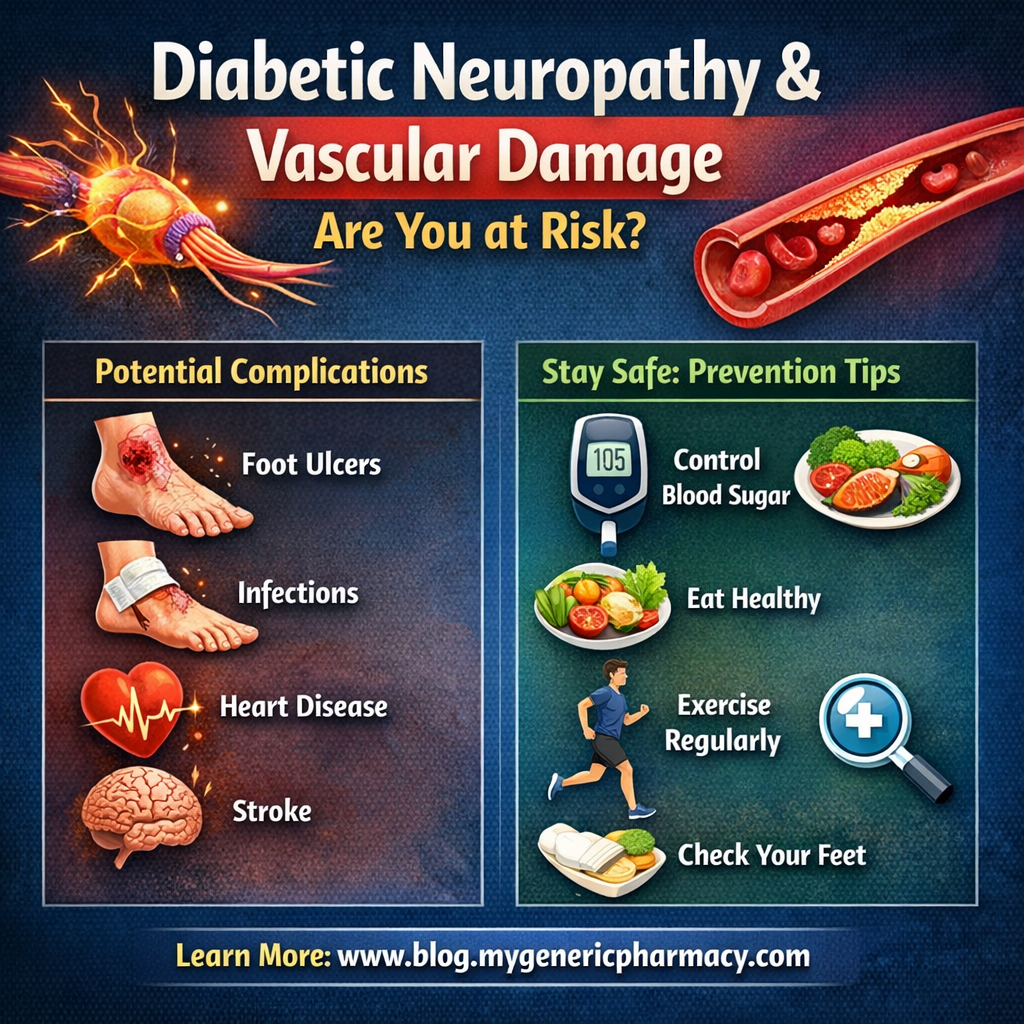
Complications: Why Diabetes Control Matters
If diabetes is not diagnosed and managed correctly, life-threatening acute events can occur, as well as progressive disability from complications. High blood-glucose levels cause progressive damage to blood vessels throughout the body.
Acute Complications
- Diabetic ketoacidosis (DKA) in type 1 diabetes
- Severe hypoglycemia (low blood sugar) from treatment
- Hyperosmolar hyperglycemic state
Chronic Complications
Cardiovascular disease: The risk of heart attack and stroke increases up to 4-fold for people living with diabetes. Diabetes can lead to coronary artery disease, heart attack, stroke, and atherosclerosis.
Kidney damage (diabetic nephropathy): The kidneys’ filtering system can be damaged, potentially leading to kidney failure.
Eye damage (diabetic retinopathy): Diabetes can damage the blood vessels of the eye, potentially leading to blindness.
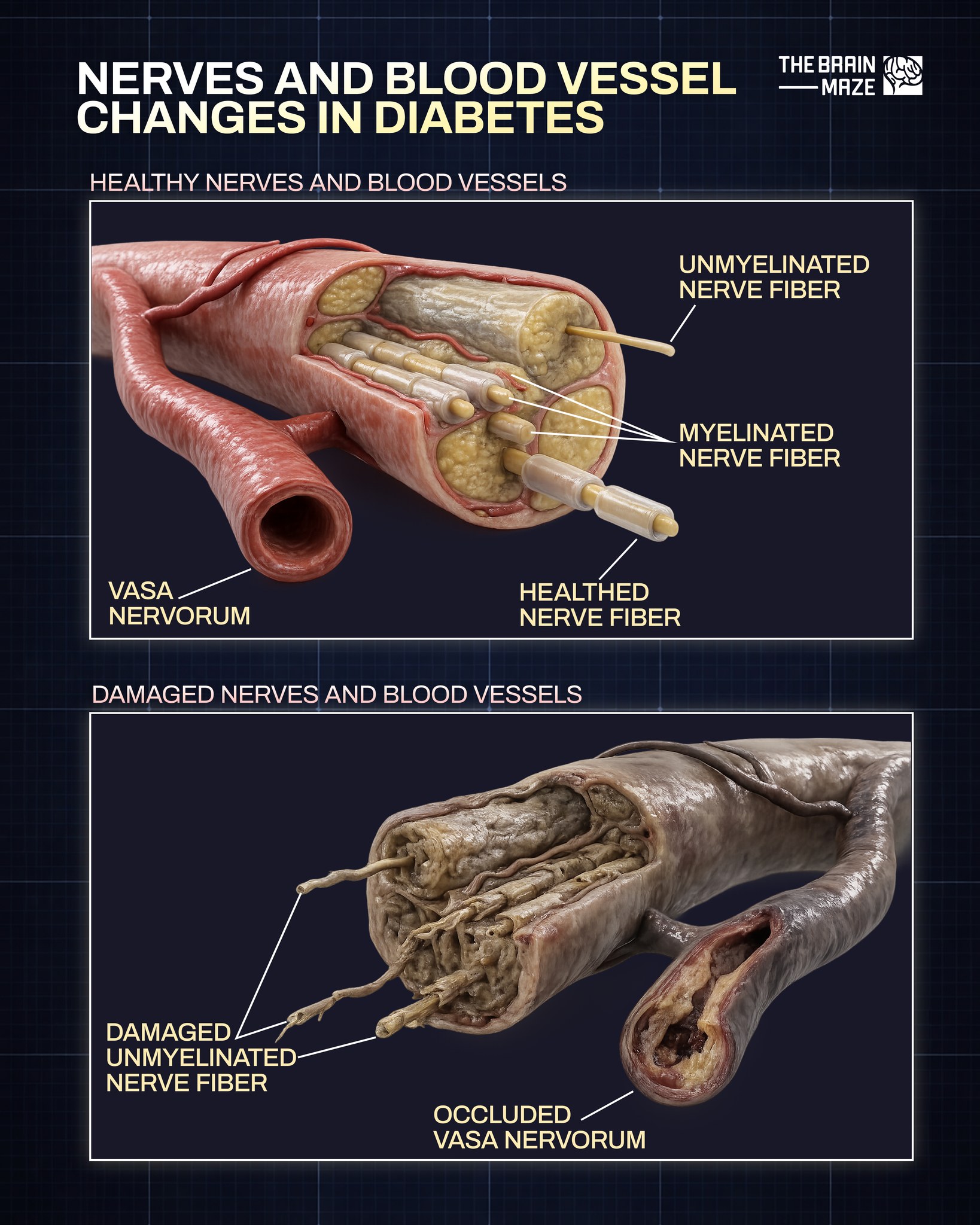
Nerve damage (diabetic neuropathy): Too much sugar can injure the walls of tiny blood vessels that nourish nerves, causing tingling, numbness, burning, or pain that usually begins in the toes or fingers and spreads upward. Damage to nerves related to digestion can cause nausea, vomiting, diarrhea, or constipation. For men, it may lead to erectile dysfunction.
Foot damage: Nerve damage or poor blood flow to the feet increases the risk of ulcers and amputations.
Other complications:
- Skin and mouth conditions (bacterial and fungal infections)
- Hearing impairment
- Alzheimer’s disease (increased risk with type 2 diabetes)
- Depression (common in both type 1 and type 2 diabetes)
Complications of Gestational Diabetes
Untreated or uncontrolled gestational diabetes can cause problems for both mother and baby :
For the baby:
- Excess growth (macrosomia), leading to a difficult birth
- Low blood sugar (hypoglycemia) after birth
- Higher risk of obesity and type 2 diabetes later in life
- Death (in severe, untreated cases)
For the mother:
- Preeclampsia (high blood pressure, protein in urine)
- Higher risk of gestational diabetes in future pregnancies
Prevention: Reducing Your Risk
Type 1 Diabetes Prevention
Type 1 diabetes cannot currently be prevented. However, research continues, and new treatments have been developed that can delay type 1 diabetes in people found to be at risk.
Type 2 Diabetes and Prediabetes Prevention
Unlike type 1 diabetes, type 2 diabetes can often be prevented or delayed through :
Lifestyle measures:
- Achieve and maintain a healthy weight: If you’re overweight, losing even 7% of your body weight can lower the risk of diabetes.
- Be physically active: Aim for 30 minutes of moderate activity on most days.
- Eat a healthy diet: Focus on fruits, vegetables, and whole grains. Limit sugars and saturated fats.
- Avoid tobacco use.
Regular screening: If you have prediabetes, have your blood sugar checked at least once a year.
Medications: For some high-risk individuals, medications like metformin may be considered.
Living Well with Diabetes
Self-Management Education and Support
Research shows that diabetes self-management education and support (DSMES) can improve A1C levels and have a positive effect on other clinical, psychosocial, and behavioral aspects of diabetes. The ADA recommends DSMES at four critical times :
- At diagnosis
- Annually
- When complicating factors develop
- When transitions in life and care occur
Mental Health and Diabetes
Living with a long-term condition can sometimes feel overwhelming. Depression symptoms are common in people with type 1 and type 2 diabetes. Health care professionals can support patients by :
- Discussing the impact of stress on health
- Engaging with patients about stressors they might experience
- Helping figure out ways to manage stress
- Normalizing the experience of stress
Regular Health Checks
If you have diabetes, your doctor will recommend regular health checks and tests :
- Blood tests to check blood glucose control and kidney function
- Blood pressure checks
- Eye tests (for retinopathy)
- Foot care checks
- Screening for other complications
Support Resources
- Diabetes organizations: National diabetes associations provide information, resources, and support services.
- Diabetes educators: These specialists can help you learn to manage your diabetes effectively.
- Support groups: Connecting with others who have diabetes can provide emotional support and practical tips.
- Technology: Continuous glucose monitors, insulin pumps, and apps can help with diabetes management.
The Emotional Impact and Stigma
It’s important to understand that a long-term condition can come with an emotional impact. People living with diabetes often find it emotionally draining to constantly correct and educate others about their condition. They may also worry about stigma.
Remember: Diabetes is a medical condition, not a character flaw. With proper support and management, people with diabetes can lead full, active, and healthy lives.
Conclusion: Hope and Progress
Diabetes is a serious condition, but tremendous progress has been made in understanding and managing it. From advances in medications and technologies to a better understanding of lifestyle factors, people with diabetes today have more tools than ever to live well.
The keys to successful diabetes management are:
- Early diagnosis through awareness of symptoms and risk factors
- Consistent management with medications, healthy eating, and physical activity
- Regular monitoring of blood glucose and complications
- Emotional support for the psychological aspects of living with a chronic condition
- Ongoing education to stay informed about new developments
Whether you have diabetes yourself or care for someone who does, remember that you are not alone. Millions of people worldwide are on this journey, and with proper care and support, diabetes can be managed successfully for a long and healthy life.
Disclaimer: This article is for educational purposes only and does not constitute medical advice. Always consult qualified healthcare providers for diagnosis and treatment of any medical condition.
References:
- World Health Organization. Diabetes fact sheet. WHO European Region.
- Diabetes UK. Differences between type 1 and type 2 diabetes.
- Healthdirect Australia. Type 2 diabetes.
- National Institutes of Health (NIDDK). How Can You Help Patients Prevent Diabetes Complications?
- Swiss Medical Network. Mayo Clinic Health Library – Diabetes.
Medications that have been suggested by doctors worldwide are available on the link below
https://mygenericpharmacy.com/category/disease/diabetes