Veins Exposed: The Hidden Highways Powering Your Body’s Life Flow
Your body is a complex network of systems working together to keep you alive and thriving. Among these, veins play a crucial yet often overlooked role. Acting as hidden highways, veins transport blood back to the heart, ensuring proper circulation and maintaining overall health. In this blog, we’ll uncover how veins work, why they matter, and how you can keep them healthy.
What Are Veins and Why Are They Important?
Veins are blood vessels responsible for carrying deoxygenated blood from various parts of the body back to the heart. Unlike arteries, which deliver oxygen-rich blood, veins work against gravity to ensure continuous blood flow.
Moreover, veins contain one-way valves that prevent blood from flowing backward. These valves are essential, especially in the legs, where blood must travel upward to reach the heart. Without properly functioning veins, circulation would become inefficient, leading to serious health issues.
How Veins Power Your Body’s Life Flow
The human body relies heavily on proper blood circulation. Veins are a key part of this system. They:
- Transport deoxygenated blood back to the heart
- Help regulate body temperature
- Support the removal of waste products from tissues
- Maintain blood pressure balance
In addition, veins work closely with muscles. When muscles contract, they squeeze veins and push blood forward. This process, known as the “muscle pump,” plays a major role in circulation, especially during physical activity.
Common Vein Problems You Should Know
Although veins are strong and resilient, they can develop problems over time. Some common vein-related conditions include:
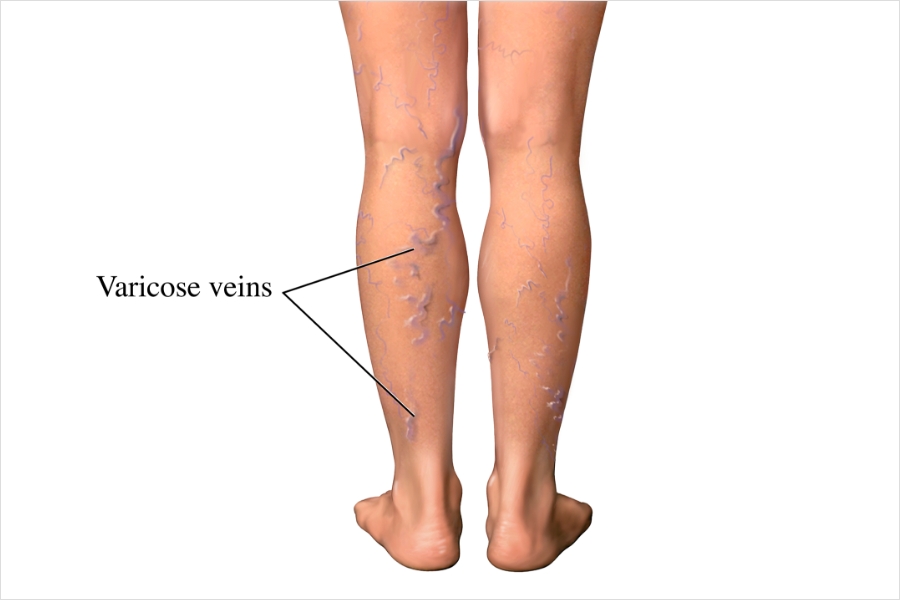
- Varicose Veins: These are enlarged, twisted veins that usually appear in the legs. They occur when vein valves become weakened, allowing blood to pool.
- Spider Veins: Smaller and less severe than varicose veins, spider veins appear as thin red or blue lines on the skin.
- Deep Vein Thrombosis (DVT): This is a serious condition in which a blood clot forms in a deep vein, typically in the legs. If untreated, it can lead to life-threatening complications.
- Chronic Venous Insufficiency (CVI): In this condition, veins struggle to send blood back to the heart, leading to swelling, pain, and skin changes.
Warning Signs of Poor Vein Health
Recognizing early symptoms can prevent complications. Watch out for:
- Swelling in legs or ankles
- Aching or heavy legs
- Visible bulging veins
- Skin discoloration
- Cramping, especially at night
If these symptoms persist, it’s important to seek medical advice.
Simple Ways to Keep Your Veins Healthy
Fortunately, maintaining healthy veins doesn’t require complicated steps. Small lifestyle changes can make a big difference.
- Stay Active: Regular exercise, such as walking or cycling, improves circulation and strengthens the muscle pump.
- Maintain a Healthy Weight: Excess weight puts pressure on veins, especially in the lower body.
- Elevate Your Legs: Raising your legs above heart level helps blood flow more easily back to the heart.
- Avoid Long Periods of Sitting or Standing: Take breaks to move around and keep blood circulating.
- Wear Compression Stockings: These help improve blood flow and reduce swelling, particularly for people at risk of vein issues.
Diet and Vein Health
What you eat also impacts your veins. A balanced diet supports circulation and vessel strength.
- Fiber-rich foods prevent constipation, reducing pressure on the veins
- Antioxidants improve blood vessel health
- Hydration keeps blood flowing smoothly
Foods like leafy greens, berries, nuts, and whole grains are especially beneficial.
When to See a Doctor
While mild symptoms can often be managed at home, some situations require medical attention. Seek help if you experience:
- Severe pain or swelling
- Sudden leg warmth or redness
- Skin ulcers or wounds that don’t heal
- Signs of blood clots
Early diagnosis and treatment can prevent serious complications.
Final Thoughts
Veins may not get as much attention as other parts of the body, but they are essential for life. These hidden highways work tirelessly to keep blood moving, remove waste, and maintain balance within your body. By understanding how veins function and taking simple preventive steps, you can protect your circulation and overall health. After all, healthy veins mean a healthier you.
References:
https://www.health.harvard.edu/blog/veins-are-a-key-player-in-the-body-heres-why-202311292997
https://my.clevelandclinic.org/health/body/23360-veins
https://pmc.ncbi.nlm.nih.gov/articles/PMC10886395/
Medications that have been suggested by doctors worldwide are available on the link below
https://mygenericpharmacy.com/category/products/blood-thinner