Skin Under Attack: How to Recognize and Treat Fungal Infections
Fungal infections are very common skin problems. They often occur in warm and humid climates. For example, they can cause itching, rashes, or skin changes. These infections can affect anyone.
In simple terms, they happen when fungi grow too much on the skin, nails, or scalp. As a result, they can spread easily. In addition, they can cause discomfort. Therefore, early treatment is important. Otherwise, the infection may get worse.
What Are Fungal Infections?
Fungi are tiny organisms that live on the skin. However, they can grow very fast in warm and moist areas. As a result, they may lead to fungal infections. In addition, the risk becomes higher in sweaty conditions.
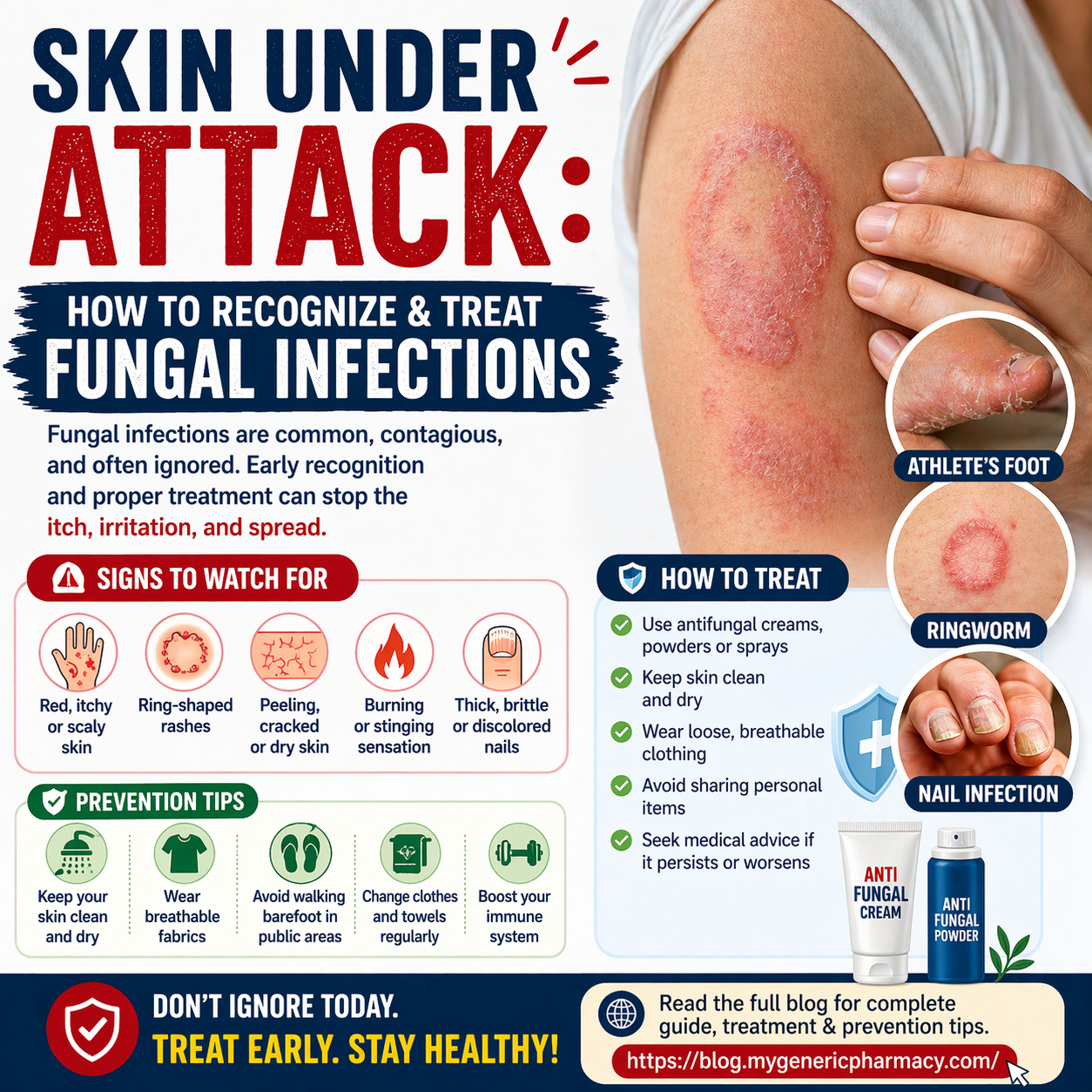
Common types include:
- Ringworm (round rash)
- Athlete’s foot (between toes)
- Jock itch (groin area)
- Nail infections (thick nails)
In addition, these infections can spread through direct contact. Moreover, they can spread through shared items. As a result, the risk of infection increases.
⚠️ Common Symptoms of Fungal Infections
If you have fungal infections, you may notice:
- Red or itchy skin
- Round rashes
- Peeling or cracked skin
- Burning feeling
- Thick or discolored nails
Moreover, ignoring these signs can make the problem worse. As a result, the infection may spread. Therefore, early action is important.
🚨 Main Causes of Fungal Infections
Several factors increase the risk.
1. Warm Climate
Fungi grow well in heat and sweat. For example, the feet and underarms are common areas. In addition, these parts stay moist for long periods. As a result, the risk of infection increases.
2. Poor Hygiene
Not keeping skin clean can increase the risk. As a result, fungi can grow faster.
3. Tight Clothing
Tight clothes trap sweat. Therefore, they create a good place for fungi.
4. Weak Immunity
A weak immune system cannot fight infections well. Consequently, the risk increases.
💊 Treatment Options
Treatment depends on the severity.
1. Topical Medicines
Creams and powders work well. For example, Clotrimazole is commonly used.
2. Oral Medicines
Doctors may give tablets for severe cases.
3. Hygiene Care
- Wash daily
- Dry skin well
- Change clothes often
4. Avoid Sharing
Do not share towels or shoes. This helps stop the spread.
🌿 Natural Remedies for Fungal Infections
Some remedies may help.
- Tea tree oil
- Aloe vera
- Coconut oil
However, these should not replace medical treatment. Instead, they can be used as support. Therefore, always follow proper medical advice.
✅ How to Prevent Fungal Infections
Fortunately, simple habits can prevent fungal infections:
- Keep skin dry
- Wear cotton clothes
- Avoid public barefoot walking
- Use antifungal powder
- Eat healthy food
As a result, your risk becomes lower. In addition, your skin stays healthy. Therefore, these habits are important.
🩺 When to See a Doctor
Seek help if:
- Infection spreads
- No improvement
- Pain or swelling appears
- You have diabetes
Early treatment helps with faster recovery.
Final Thoughts
Fungal infections may seem minor. However, they can become serious if ignored. Over time, they may cause discomfort. Therefore, early recognition is important.
In addition, proper treatment and good hygiene help a lot. By doing this, you can protect your skin. As a result, your overall health improves.
🧾 Conclusion
In conclusion, fungal infections are common. However, they are easy to treat. If ignored, they can get worse. Therefore, early care is important.
In addition, good hygiene helps prevent them. As a result, your skin stays healthy. Ultimately, simple habits make a big difference.
References:
- World Health Organization. (2022). Skin infections and global health burden.
- Centers for Disease Control and Prevention. Fungal Diseases Overview.
- Mayo Clinic. Fungal Infection: Symptoms and Causes.
- National Institutes of Health. Dermatophyte infections and treatment.
- American Academy of Dermatology. Fungal Skin Infections: Diagnosis and Care.
Medications that have been suggested by doctors worldwide are available on the link below
https://mygenericpharmacy.com/category/disease/fungal-infection