Joint Pain & Bone Health: What You Need to Know to Stay Active
Joint pain and poor bone health can limit mobility and reduce quality of life. In 2026, more people are focusing on staying active and preventing long-term issues. Understanding how your bones and joints work—and how to care for them—can help you remain strong, flexible, and pain-free.
What Are Bones and Joints?
Your bones form the structure of your body, while joints connect bones and allow movement. Healthy joints rely on cartilage, ligaments, and fluid to function smoothly.
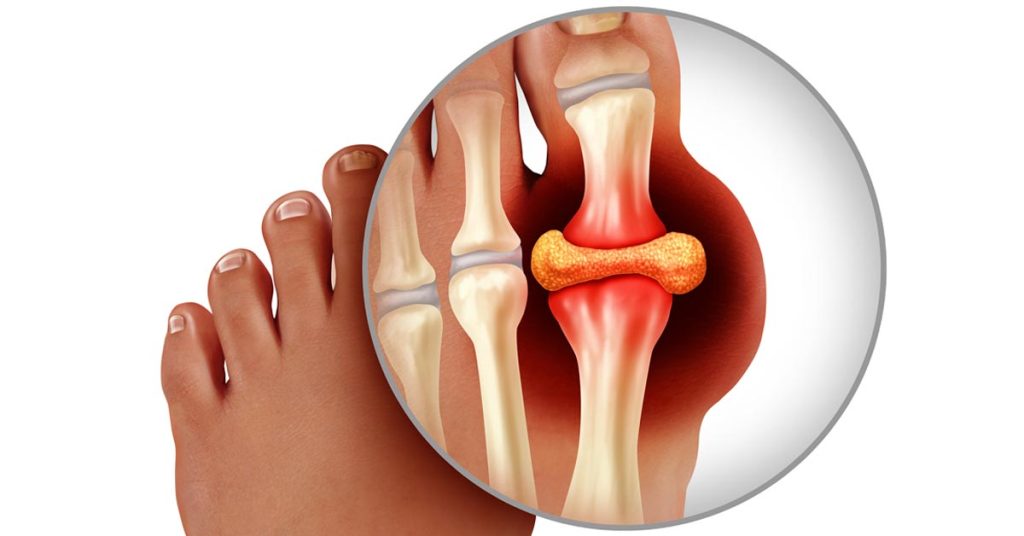
Conditions like Osteoarthritis and Osteoporosis are common causes of joint pain and bone weakness, especially as people age.
Common Causes of Joint Pain
Joint pain can occur for many reasons, ranging from temporary strain to chronic conditions.
- Aging: Natural wear and tear on joints
- Injuries: Sprains, fractures, or overuse
- Inflammation: Conditions like arthritis
- Poor posture: Adds stress to joints
- Lack of activity: Weakens muscles and joints
Identifying the cause is essential for effective treatment.
Signs You Should Not Ignore
Early symptoms of joint and bone problems should never be overlooked.
- Persistent joint pain or stiffness
- Swelling or redness
- Reduced range of motion
- Weak or brittle bones
- Pain during movement
If these symptoms continue, seeking medical advice is important.
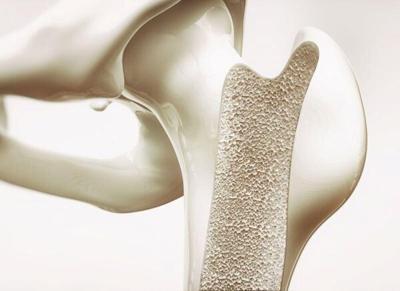
Why Bone Health Matters
Strong bones support your body and protect vital organs. However, bone density naturally decreases with age, increasing the risk of fractures.
Maintaining bone health is crucial, especially for older adults and women after menopause, who are at higher risk of bone loss.
How to Keep Your Bones and Joints Healthy
1. Stay Physically Active
Regular exercise strengthens muscles and improves joint flexibility. Activities like walking, yoga, and strength training are highly beneficial.
2. Eat a Nutrient-Rich Diet
Calcium and vitamin D are essential for bone health. Include dairy products, leafy greens, and fortified foods in your diet.
3. Maintain a Healthy Weight
Excess weight puts additional stress on joints, especially knees and hips.
4. Practice Good Posture
Proper posture reduces strain on your joints and prevents long-term damage.
5. Stay Hydrated
Joint lubrication depends on proper hydration, which helps reduce stiffness.
Lifestyle Habits That Harm Bone and Joint Health
Certain habits can weaken bones and worsen joint pain:
- Smoking
- Excessive alcohol consumption
- Sedentary lifestyle
- Poor nutrition
Avoiding these habits can significantly improve your long-term health.
While mild joint pain may improve with rest, some situations require medical attention:
- Severe or persistent pain
- Joint deformity
- Sudden swelling
- Difficulty walking
Early diagnosis can prevent complications and improve treatment outcomes.
Treatment Options for Joint Pain
Treatment depends on the cause and severity of the condition.
- Medications: Pain relievers and anti-inflammatory drugs
- Physical therapy: Improves strength and flexibility
- Lifestyle changes: Diet and exercise adjustments
- Surgery: In severe cases, joint replacement may be needed
A personalized approach is the most effective way to manage joint issues.
Conclusion: Stay Active, Stay Strong
Joint pain and bone health are closely connected to your overall well-being. By adopting healthy habits, staying active, and addressing symptoms early, you can maintain mobility and enjoy a better quality of life.
In 2026, the goal is simple—protect your bones, care for your joints, and stay active for years to come.
References:
- World Health Organization – Musculoskeletal health guidelines
- Centers for Disease Control and Prevention – Arthritis and joint health resources
- International Osteoporosis Foundation – Osteoporosis prevention and management
- Mayo Clinic – Joint pain causes and treatments
Medications that have been suggested by doctors worldwide are available on the link below
https://mygenericpharmacy.com/category/products/pain-relief