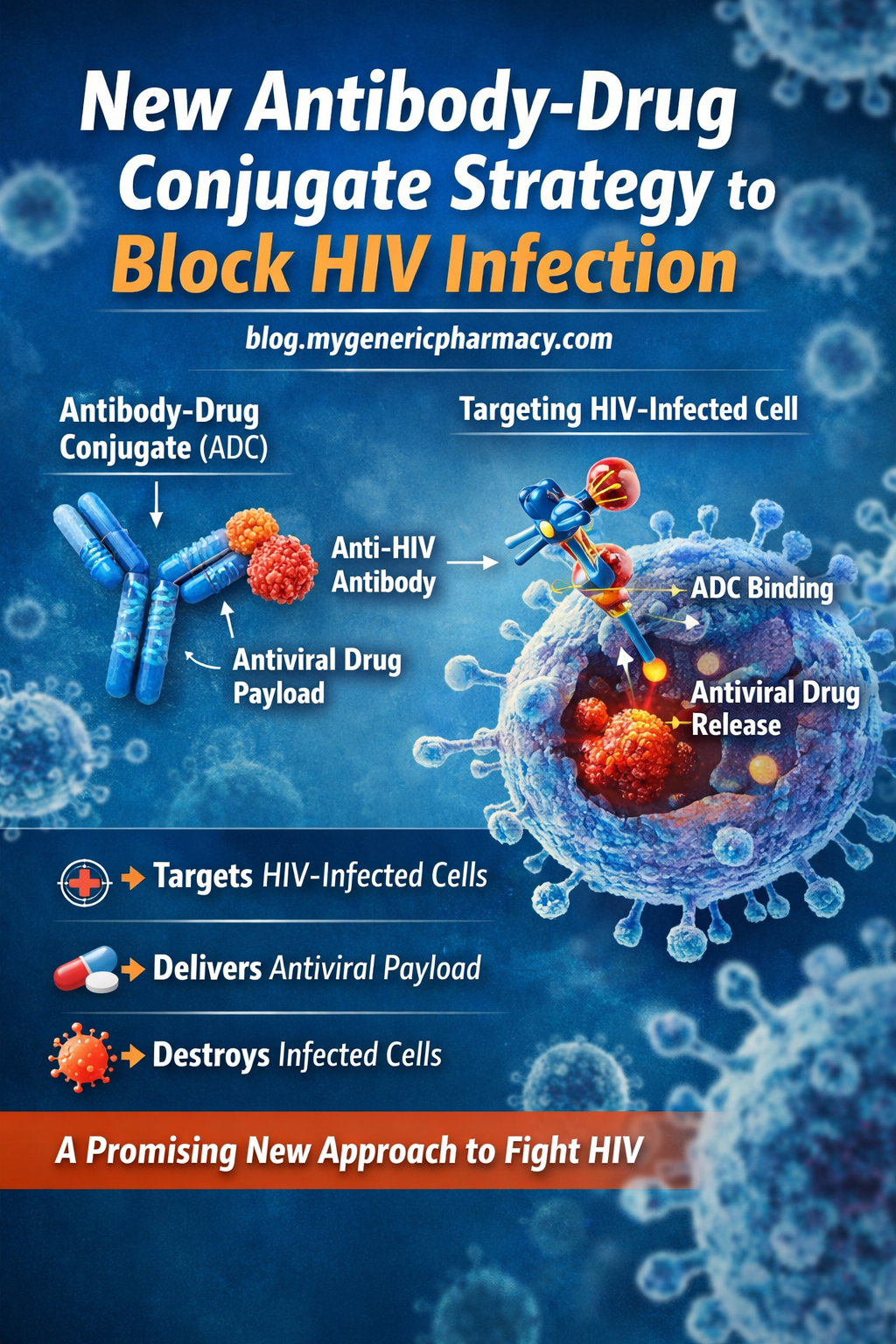
Metformin, a common diabetes drug, was tested by researchers to see if it could stop lengthy COVID.
Metformin can cut down lengthy COVID diagnosis by 40%, according to their research. If these results apply to the general population, more research is required.
Long COVID is characterised by continuous health issues that continue even after a COVID-19 diagnosis and cannot be attributed to any other causes.
The duration of symptoms might range from weeks to years. Long COVID has been associated with more than 200 symptoms, from exhaustion and nausea to memory loss, stomach discomfort, and dyspnea or difficulty breathing.
What causes lengthy COVID has been the subject of several different theories. Mechanistic research, however, are still in their early stages. The illness is still in its early stages of development, as are treatments and prevention strategies.
The coronavirus that causes COVID-19, SARS-CoV-2, is currently the greatest strategy to prevent lengthy COVID, according to the Centres for Disease Control and Prevention (CDC). This can be done, for example, by staying current on vaccines.
The quality of life and reduction of long-term handicap among patients could be improved by measures to prevent protracted COVID after contracting COVID-19.
Three widely used medications were recently investigated for their ability to prevent extended COVID.
They discovered that lengthy COVID was considerably less likely to occur in participants taking metformin compared to those taking a placebo. A common diabetes drug called metformin raises insulin sensitivity to reduce blood sugar levels.
Metformin may reduce the occurrence of long-term COVID.
It was a phase 3 randomised clinical trial. 1,126 individuals with COVID-19 symptoms and a positive PCR or antigen test for this viral infection, ranging in age from 30 to 85 years, were enrolled by the researchers.
The patients had either fat or overweight, which increased their likelihood of developing severe COVID even though they were not hospitalised for COVID-19.
The individuals were randomly assigned to one of six groups, each of which received a different dosage of metformin for 14 days, ivermectin for 3 days, fluvoxamine for 14 days, and placebo. Fluvoxamine is used to treat obsessive-compulsive disorder (OCD), and ivermectin is an antiparasitic medication.
For ten months, the subjects were monitored. Throughout the follow-up period, they were questioned multiple times about whether they had obtained a medical provider’s diagnosis of extended COVID.
After 300 days of follow-up, 8.3% of patients overall reported a lengthy COVID diagnosis. Only 6.3% of patients who took metformin, as opposed to 10.4% of those who received a placebo, experienced lengthy COVID.
In comparison to a placebo, ivermectin and fluvoxamine had no effect on the incidence of long-term COVID.
The Safe Drug Metformin Has Proven Antiviral Effects
Based on the knowledge that metformin is safe and has proven anti-inflammatory and antiviral capabilities, the study team pursued it as a potential long-COVID treatment.
Hector Fabio Bonilla, MD, is the co-director of the Stanford Post-Acute COVID-19 Syndrome Clinic and has observed laboratory test outcomes that support metformin’s potential to lessen antiviral and anti-inflammatory activities that can result in thrombosis (when blood clots block blood arteries) and lung harm.
Dr. Bonilla, who is also a clinical associate professor of infectious diseases at Stanford University, adds, “Plus, this drug is relatively safe, with no increased risk of hypoglycemia low blood sugar and no increased risk of lactic acidosis lactic acid buildup related to low oxygen levels.” There is no need to cease taking metformin before surgery because it is safe to take during pregnancy, breastfeeding, and in individuals with renal failure.
Underlying processes
We discussed how metformin may have decreased long COVID risk with Dr. Mark Guido, an endocrinologist from Novant Health Forsyth Endocrine Consultants in Winston Salem, NC, who was not involved in the study.
It is difficult to say because we still don’t fully comprehend extended COVID, but it might be connected to lowering inflammation, he suggested. Additionally, metformin has been demonstrated to potentially lessen severe COVID and to halt the reproduction of the [SARS-CoV-2] virus in a lab setting, both of which may also be involved.
We also discussed how metformin may have decreased long COVID risk with Dr. Daniel Kim, a board-certified family doctor of Medical Offices of Manhattan who was not part in the study.
He concurred that it is still unknown exactly how certain things work. Nevertheless, he added that earlier research suggests that metformin has an antiviral effect by preventing viral multiplication.
Do all people fall within the study’s conclusions?
Dr. Guido responded to a question concerning the study’s limitations by saying, “Since our understanding of long COVID is still evolving, there were no specific diagnostic criteria used to determine who did or did not qualify as having long COVID.”
“The trial was also restricted to participants who were overweight or obese and were not currently on metformin. It is unknown if people who are already on metformin for other disorders or who have a normal weight will experience the same effects from metformin,” he added.
The trial was limited to examining the use of metformin to stop long-term COVID during a patient’s initial COVID infection. It is uncertain whether metformin would guard against extended COVID if a patient had previously contracted COVID-19, he continued.
According to Dr. Kim, “It is also unknown if [the results] can be generalized to early outpatient treatment of COVID-19 patients who were previously diagnosed with COVID-19 infection.”
Avoiding prolonged COVID
The results, according to Dr. Guido, could have a significant impact on short COVID prevention.
“Long COVID is turning into a public health emergency. Long-term public health would greatly benefit if it could be successfully decreased by a cheap, well-tolerated, and easily accessible medicine like metformin,” he said.
Dr. Kim concurred that the results are encouraging. He did point out that additional research is required to evaluate whether metformin is as effective for the broader populace.
REFERENCES:
For Diabetes medications that have been suggested by doctors worldwide are available here https://mygenericpharmacy.com/index.php?therapy=13