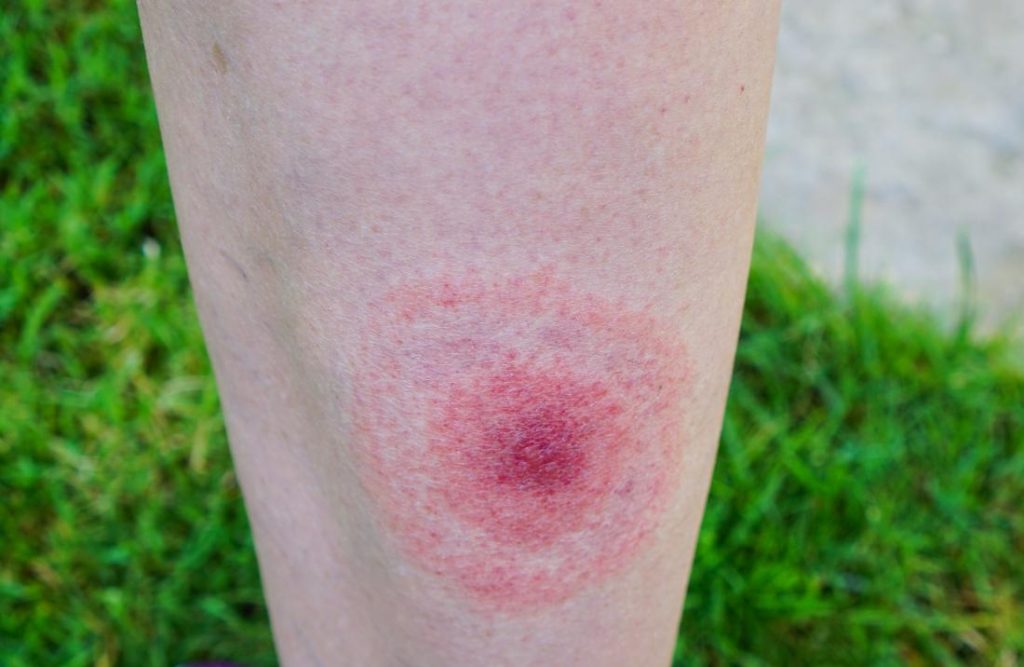
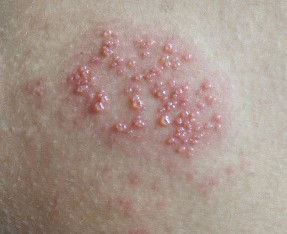
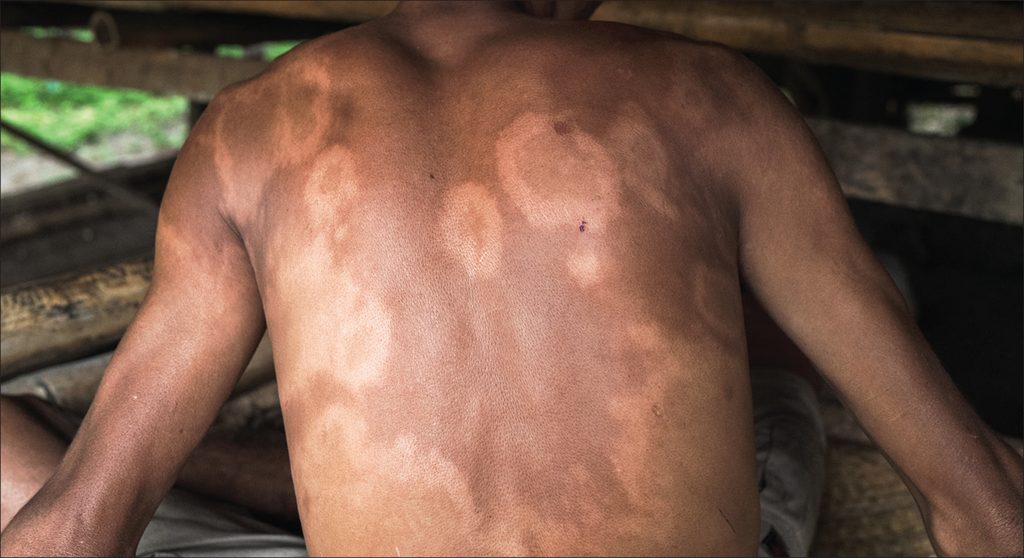
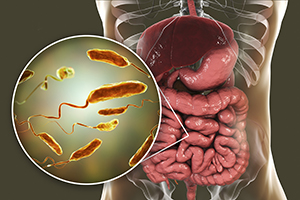
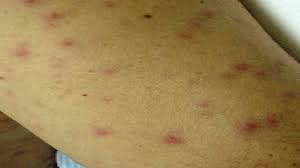
Risk factors involved with Primary immunodeficiency disease
Immune deficiencies make it difficult for your body to fight off illnesses and infections. You are more likely to contract viruses and bacterial illnesses if you have this kind of condition.
Disorders of the immune system can be either inherited or acquired. You are born with a congenital, or primary, disease. A secondary or acquired disorder is one that develops later in life. Congenital disorders are less frequent than acquired disorders.
The following organs are part of your immune system:
- spleen
- tonsils
- blood marrow
- lymph glands
Lymphocytes are processed and released by these organs. These are T cells and B cells, two types of white blood cells. Antigen-based intruders are fought by B and T lymphocytes. B cells release antibodies that are tailored to the illness your body has identified. Some T cells eliminate abnormal or alien cells.
Your B and T cells may need to defend themselves against various antigens, for instance:
- bacteria
- viruses
- melanoma cells
- parasites
Your body’s capacity to fight itself against these antigens is interfered with by an immunodeficiency condition.
What is a weak immune system?
You are immunocompromised if your immune system is impaired. This indicates that, compared to healthy individuals, your body is less capable of fending off viruses or diseases.
A weakened immune system can momentarily be brought on by treatments like anticancer therapies and radiation therapy, despite the fact that it is primarily brought on by certain illnesses, starvation, and specific genetic problems.
A stem cell or organ transplant may also momentarily impair your immune system.
Signs of an immunodeficiency disorder
Immunodeficiency illnesses come in many different shapes and sizes. Each illness has distinct symptoms that may be recurrent or persistent. There are, however, a few red flags that suggest your immune system may be malfunctioning.
Those who suffer from immunodeficiency disorders frequently get infections of certain illnesses, such as:
- red eye
- sinus problems
- thrush
- colds
- persistent gum disease (gingivitis)
- pneumonia
- Candida infections
Immunodeficiency condition sufferers may experience chronic stomach pain as well as weight loss over time. Your doctor may do an immunodeficiency disorder test if you notice that you are susceptible to illnesses and viruses, and that you have trouble recovering from them.
Types of immunodeficiency disorders
When the immune system is not functioning as it should, an immune deficiency disease or disorder develops. It is referred to as primary immunodeficiency disease if you are born with a deficiency that has a hereditary aetiology. Primary immunodeficiency disorders number over 200.
Primary immunodeficiency disorders include, for example:
- common variable immunodeficiency (CVID)
- severe combined immunodeficiency (SCID), which is also known as alymphocytosis
- chronic granulomatous disease (CGD)
When your body is weakened by an external factor, such as a chemical or virus, secondary immunodeficiency problems develop. A secondary immunodeficiency condition can result from the following:
- a lot of burns
- chemotherapy
- radiation
- diabetic nephropathy
- malnutrition
Secondary immunodeficiency disorders include, for example:
- AIDS
- immune system malignancies, such as leukaemia
- immune-complex diseases, like viral hepatitis
- multiple myeloma (cancer of the plasma cells, which produce antibodies)
Causes of immunodeficiency disorders
Numerous primary immunodeficiency diseases are inherited and are acquired from either one or both parents. Many of these immune system flaws are brought on by issues with the DNA, which serves as the body’s blueprint for genetic construction.
More than 300 different primary immunodeficiency illnesses have been identified so far, and new ones are constantly being discovered. Based on whatever immune system component is impacted, they can be roughly divided into six groups:
- Lack of B cells and antibodies
- defects in T cells
- a combined lack of B and T cells
- flawed phagocytes
- Deficits in the complement
- Unknown (idiopathic)
Risk factors
A larger risk of acquiring primary immunodeficiency disorders in oneself exists in those with a family history of such conditions. An additional immunodeficiency condition can result from anything that impairs your immune system. As an illustration, exposure to HIV-infected bodily fluids or organ excision and replacement are both potential causes.
Additionally, ageing can impair your immune system. Some of the organs that make or process white blood cells decrease and perform less effectively as you age. Proteins are essential for maintaining immunity. Your immune system may become weakened if you don’t consume enough protein.
While you sleep, your body also generates proteins that aid in the body’s ability to fight infections. Because of this, getting too little sleep can weaken your immune system. Additionally, cancer and chemotherapy medications can lower your immunity.
Prevention of immunodeficiency disorders
There is no method to prevent primary immunological illnesses because they are brought on by genetic alterations. However, there are precautions you can do to avoid infections if you or your child has a compromised immune system:
- Maintain proper hygiene. Use a light soap to wash your hands after using the restroom and before eating.
- Maintain good oral hygiene. At least twice a day, brush your teeth.
- Proper diet, An illness can be avoided with a healthy, balanced diet.
- Be active physically. Your whole health depends on maintaining a healthy lifestyle. Find out what activities are suitable for you by asking your doctor.
- Get adequate rest. Try to get the same amount of sleep each night and try to go to bed and wake up at the same time each day.
- Stress management. According to certain research, stress may weaken your immune system. Massage, meditation, yoga, biofeedback, or hobbies can help you manage your stress. Figure out what works for you.
- Prevent exposure. Avoid crowds and persons who have colds or other diseases.
- Consult your doctor regarding vaccines. Learn which ones you ought to have.