How and why does exercise improve cognitive function?
The molecular mechanisms by which exercise enhances cognition were studied. They discovered that muscular contractions emit chemical signals that promote neuronal development and activation.
They also discovered that astrocytes, which act as support cells, protect neurons from excessive electrical signalling when they are exposed to chemical signals from muscle cells.

To determine whether these findings hold true for humans, more research is required. The maintenance of both physical and mental health requires exercise. Even if it is started later in life, according to studies, it has a good impact on health.
Some people believe that exercise enhances cognition by causing long-term alterations in the hippocampus, such as increased volume and faster pace of neuron production. However, it is still unclear exactly how exercise affects the hippocampus.
Researchers may be able to reverse-engineer treatments for cognitive diseases like dementia if they have a better understanding of how exercise increases hippocampus size and functionality.
In order to comprehend how exercise alters hippocampus cells, researchers have conducted a number of in vitro tests, or investigations in cell cultures.
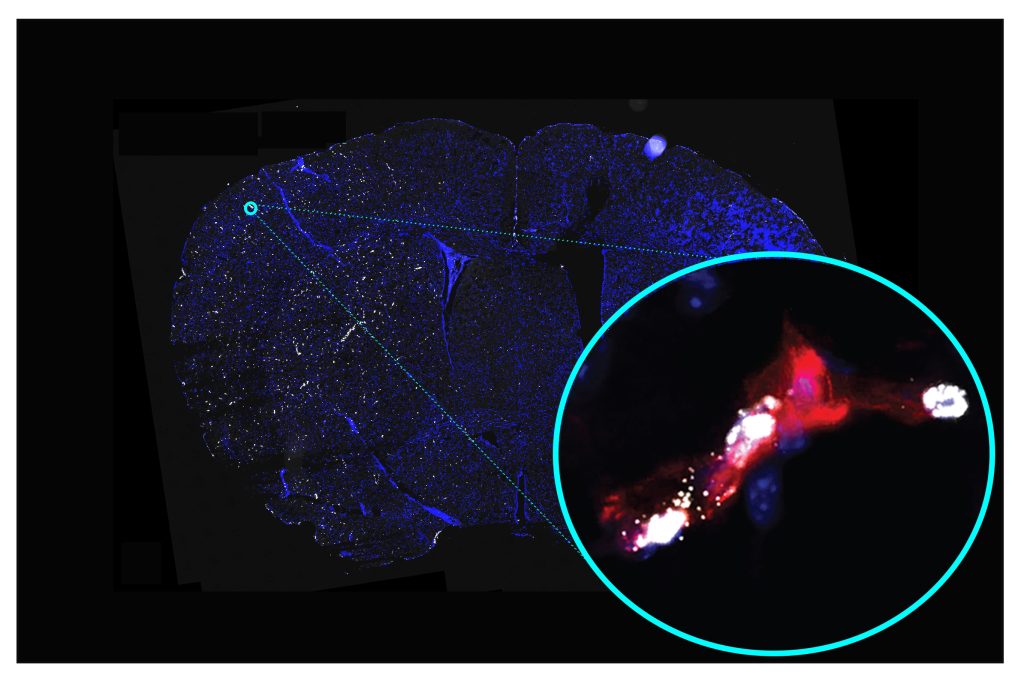
They discovered that hippocampus cells grew and fired more electrical signals as a result of chemical signals generated by muscles that were contracting. Additionally, they discovered that astrocytes, which are support cells, control neuronal activity and growth for optimal brain function.
According to Ryan Glatt, senior brain health coach and director of the FitBrain Programme at Pacific Neuroscience Institute in Santa Monica, California, who was not involved in the study, “the implications support prior findings from other studies, which is that exercise, including muscle-strengthening exercises like resistance training, can have a positive impact on brain function.”
How muscles may ‘speak’ to the brain
The tiny muscle progenitor cells were taken from mice and grown in Petri dishes for the investigation. They started to contract and release chemical signals into the cell culture once they reached adulthood.
The scientists then transferred the substances that had been in the mature muscle cell culture to astrocytes and hippocampus neurons in a separate dish.
They monitored cell proliferation using immunofluorescence and calcium imaging, and they recorded neural activity using multi-electrode arrays. In the end, they discovered that hippocampal neurons and astrocyte numbers grew by 1.4 and 4.4 times, respectively, in response to chemical signals from the muscle cells.
The development of mature hippocampal neural networks, which are composed of cells that fire synchronously, was hastened by the addition of muscle cell cultures.
The next step was to investigate the impact of astrocytes on the combination. They did this by observing what happened when astrocytes were removed from cell cultures containing mature muscle and hippocampus cells.
They observed that the neurons fired even more electrical signals as a result, indicating that astrocytes may assist regulate and coordinate neural activation patterns. Further studies revealed that the observed alterations in hippocampus cultures required muscular contractions.
Hippocampal cells no longer showed the same amounts of neuronal firing when muscle cells were stopped from contracting, but synchronous firing was intact.
The study authors remarked that this indicates that muscle contractions or exercise release substances that are not released by stationary cells. They came to the conclusion that their research offers fresh perspectives on how exercise might help hippocampus function.
Dementia risk and exercise
We enquired about how exercise can lower the incidence of dementia from Dr. Rong Zhang, a neurologist from the O’Donnell Brain Institute at UT Southwestern who was not involved in the study.
He pointed out that extensive clinical trials are still needed to determine whether this is the case, and that additional study should look at the underlying molecular mechanisms as well.
Meanwhile, Dr. Bennett pointed out that earlier studies demonstrate that exercise lowers the risk of dementia by:
- increasing the brain’s blood flow
- inflammation reduction
- lowering anxiety
- enhancing sleep
- making it easier to keep healthy body weight.
We also had a conversation with Dr. Romnesh de Souza, an interventional and consulting neurologist at Health City Cayman Islands who was not associated with the study.
He stated, regular aerobic exercise, such as walking, power walking, swimming, or riding an exercise bike, should be done for 20 to 30 minutes each day. 70% of your maximum heart rate should be your target. Subtract your age from 220 to get a ballpark idea of your maximal age-related heart rate. It has been demonstrated that this practice reduces dementia by 30–35%.
Non verified finding in humans
“Rats were used in an in vitro study that used cell culture. If these findings apply to individuals, more research will be necessary to determine,” Dr. Zhang said in response to the study.
Although she was not involved in the study, Dr. Lauren Bennett, director of neuropsychology at the Pickup Family Neurosciences Institute at Hoag Memorial Hospital Presbyterian, noted that the research “was only conducted for a short period of time, and it is not clear whether the findings would be the same over a longer period of time.”
Ways to fight rising cases of dementia
Among the largest risks to the country’s public health are Alzheimer’s disease and other types of dementia.
This study focused on assisting persons with mild cognitive impairment rather than directly addressing Alzheimer’s disease. It has been demonstrated that dementia brought on by Alzheimer’s disease or other neurological diseases is more likely to occur in people with mild cognitive impairment.
The prevention of Alzheimer’s disease and other types of dementia has been a focus of research. Right now, there is no remedy. The need for this research has increased as the population of America ages quickly. Every day, more than 10,000 people reach the age of 65.
Alzheimer’s disease and associated dementias cause one in three senior deaths and claim more lives than breast and prostate cancers put together. The Alzheimer’s Association estimates that about 13 million Americans over 65 will have Alzheimer’s disease by the year 2050, up from the current total of more than 6 million.
Alzheimer’s disease and other dementia-related fatalities increased by 16% during the pandemic.
Upcoming applications
In spite of this, Dr. Bennett stated that “the results of this study provide further evidence of the importance of exercise, at any point in life, in supporting hippocampal plasticity to combat hippocampal atrophy, which is a hallmark of Alzheimer’s disease.”
In the future, she said, “studies like this could play a crucial role in aiding us in optimizing exercise programs to support cognitive health.” Dr. de Souza continued by saying that the results may also help in the creation of fresh therapies for cognitive impairment.
These results suggest that it may someday be possible to’reverse engineer treatments to mimic pro-cognitive effects of exercise in the absence of physical activity.’ The possibility of using this to slow or stop the process of cognitive deterioration in dementia patients is also intriguing, he added.
REFERENCES:
- https://www.medicalnewstoday.com/articles/how-and-why-does-exercise-improve-cognitive-function
- https://www.healthline.com/health-news/can-aerobic-exercise-improve-cognitive-function-and-decrease-alzheimers-disease-risk
- https://www.cdc.gov/nccdphp/dnpao/features/physical-activity-brain-health/index.html
- https://www.clinicbarcelona.org/en/news/how-does-physical-activity-affect-the-brain
For Cognitive disease medications that have been suggested by doctors worldwide are available here https://mygenericpharmacy.com/index.php?cPath=77_478