Treating hypertension with help of the ultrasonic device.
Introduction
The findings of a recent meta-analysis of prior studies looking into a novel method of blood pressure control seem promising. It explains a treatment that “mutes” overactive kidney nerves, a sign of hypertension frequently observed in middle-aged adults.
Participants’ blood pressure was dramatically reduced after the procedure, dropping by an average of 8.5 millimeters of mercury (mmHg). Follow-ups two months later and three years later supported the effectiveness of this advantage.
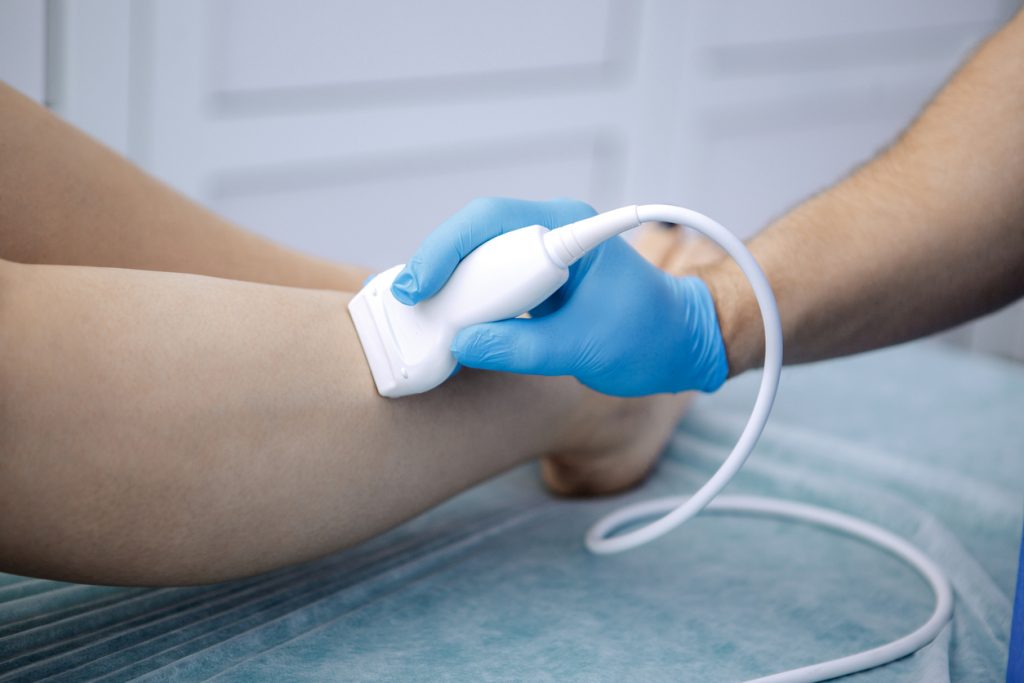
One of the primary causes of death on a global scale is hypertension or high blood pressure. In addition to heart, brain, and renal disorders, it can cause strokes. Since an estimated 46% of people with hypertension are unaware that they have it, it is frequently referred to as the “silent killer”.
Many hypertension medications, may be helpful in addition to a healthy lifestyle and dietary adjustments in managing the illness. Many folks find this to be adequate. Nonetheless, some people’s blood pressure continues to be consistently high.
Reports
According to a recent meta-analysis, the 506 hypertensive participants in three randomized clinical trials had considerably lower blood pressure when therapeutic ultrasonography was used to reduce kidney-nerve hyperactivity.
The exact etiology of hypertension is unknown. Scientists speculate that it may be a result of a mix of genetics, lifestyle, aging, and other processes.
Middle-aged hypertension is typically accompanied by hyperactive renal nerves, which can raise blood pressure in several different ways. It could cause salt and water retention as well as the production of hormones that raise blood pressure.
Even though there are many different medications for treating hypertension, none explicitly target this renal overactivity. So, the “renal denervation” ultrasound approach investigated in the present study provides clinicians with an extra instrument. Thi was made to support patients in maintaining their health.
Researchers from the Université de Paris in France and Columbia University in New York City carried out the study. You can find it in JAMA Cardiology.
How blood pressure is measured?
Millimeters of mercury, or mmHg, is used to measure blood pressure. This is because early precise blood pressure gauges and some contemporary systems rely on mercury.
Two blood pressure readings are usually displayed, one above the other or to the left of the other. Systolic blood pressure, or the pressure the heart puts off when pumping blood, is the first value. The pressure in arteries between heartbeats is shown by the second value, called the diastolic value.
The American Heart Association defines good blood pressure as having a systolic reading of less than 120 mmHg over a diastolic reading of less than 80 mmHG. A value of 130–139/80–89 mmHG indicates stage 1 hypertension. Higher results indicate hypertension in stage 2.
The current study discovered that renal denervation dramatically decreased participants’ blood pressure, by 5 to 10 mmHG, with an average decrease of 8.5 mmHg.
kidney nerves and high blood pressure
It is believed that overactive renal nerves induce water and sodium retention and produce hormones that can elevate blood pressure. They are a contributing factor in the development of hypertension in middle age. As blood arteries stiffen in older adults, hypertension frequently develops.
Antihypertensive medications lower blood pressure in a variety of methods, such as by dilation of blood vessels, removal of extra fluid, or blockage of hormones that elevate blood pressure. Yet, none of these drugs specifically target the renal nerves.
By calming hyperactive nerves in the renal artery, ultrasound treatment blocks the signals that cause hypertension. A thin catheter that is placed into a vein in the wrist or leg and sent to the kidney delivers the therapy to the nerves.
Renal denervation
A tiny catheter that is placed into a vein in the leg or wrist and threaded into the kidney makes up the renal denervation device addressed in the study. During the operation, ultra-high-frequency sound waves are used to treat the kidney’s nerves. This causes minute amounts of scar tissue to form, which reduces the nerve activity. “Ablation” is the name of this procedure.
Lead author Dr. Ajay J. Kirtaine predicted that the surgery would be performed as an outpatient, similar to cardiac catheterization.
“Ultrasound-renal denervation’s ablation portion is less than one minute, and the whole procedure is less than an hour, with conscious sedation/local anesthetic,” he said.
In the research, participants were divided into two groups: the ultrasound denervation group and the control group, which had a sham operation with no therapeutic benefit.
The number of participants in the study arm who received the therapy to lower blood pressure to 135/85 was twice as high. This outcome was the same in all three investigations, which included a population of different racial backgrounds, indicating the technique is probably valuable to many people.
The investigations indicated that the reduction in blood pressure persisted for at least 2 months following the operation and that participants’ blood pressure was improved. The result of the surgery “appears to be durable with follow-up out to 3 years,” according to Dr. Kirtaine.
Not yet, at least not for everyone.
The device is experimental so far, having not acquired permission for usage in the United States. The study’s authors plan to apply it to people whose blood pressure is still uncontrolled despite modifying their lifestyles and taking medication.
Dr. Jayne Morgan, a cardiologist who was not involved in the study, concurred and viewed the procedure as perhaps a secondary treatment rather than a first-choice therapy. But she noted, “I envision that this might certainly be reversed in the future with continued trials and information/data.
According to Dr. Morgan, the surgery may be especially beneficial for Black people and other minorities who have high rates of hypertension and heart disease.
This is a terrific reason why Black volunteers should be recruited, she said, since it may offer a more long-lasting option for blood pressure control in the future. 17% of participants in the meta-analysis were Black Americans.
Dr. Devin Kehl, who was not involved in the research, issued a warning: “The trials have been quite limiting in their inclusion and exclusion criteria,” despite the fact that the technique has an outstanding long-term safety profile and is probably safe.
REFREENCES:
- https://www.news-medical.net/news/20230228/Ultrasound-device-may-help-some-hypertensive-patients-to-keep-blood-pressure-under-control.aspx
- https://www.medicalnewstoday.com/articles/medical-myths-all-about-hypertension
- https://www.miragenews.com/ultrasound-device-could-treat-hypertension-study-956689/
- https://www.upi.com/Health_News/2023/02/28/ultrasound-device-blood-pressure/6651677598730/
For more details, kindly visit below.