Explore the body functions affected by Multiple Sclerosis.
Your nerves are impacted by multiple sclerosis, which manifests as symptoms including weariness, trouble walking, and speech problems. There is currently no cure, however there are a number of therapies that can help you manage the symptoms.
A persistent disorder affecting your central nervous system is called multiple sclerosis (MS). Your immune system destroys myelin, the covering that surrounds nerve fibres, when you have MS.
Inflammation and transient lesions are brought on by MS. Additionally, it may result in long-lasting lesions brought on by scar tissue, making it challenging for your brain to communicate with the rest of your body. MS cannot be cured, but symptoms can be controlled.
What is Multiple Sclerosis?
Although they are unsure of the actual cause of MS, researchers think it is an autoimmune condition that affects the central nervous system (CNS). The immune system assaults healthy tissue when a person has an autoimmune disease, just as it could attack a virus or bacteria.
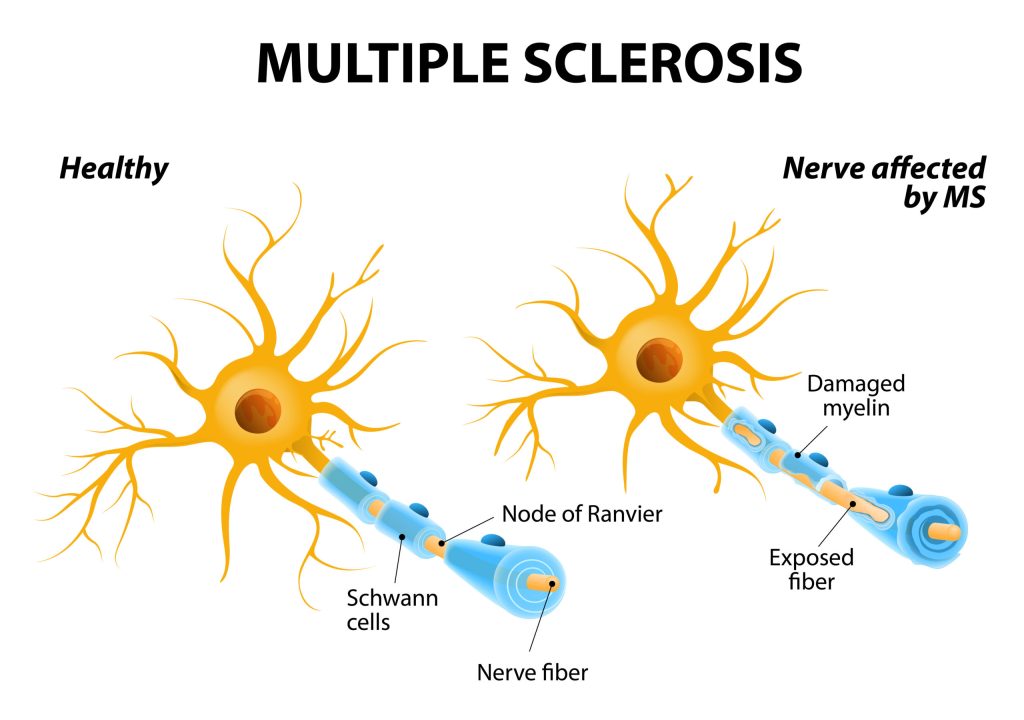
In MS, inflammation results from the immune system attacking the myelin sheath, which covers and shields the nerve fibres. The nerves’ ability to swiftly and effectively conduct electrical signals is enabled by myelin.
“Scar tissue in numerous sites” is what multiple sclerosis signifies. Sclerosis, or a scar, results from the myelin sheath disappearing or being damaged in several places. These regions are also referred to by doctors as plaques or lesions. They mostly impact:
- the cerebral stem
- the cerebellum, which controls balance and movement coordination,
- spinal cord
- ocular nerves
- Some brain areas have white matter.
Nerve fibres may rupture or suffer damage as more lesions appear. The electrical impulses from the brain do not reach the target nerve smoothly as a result. This implies that the body is unable to do some tasks.
Types of MS and stages
Multiple sclerosis comes in four different forms:
- Clinically isolated syndrome (CIS): When someone experiences their first bout of MS symptoms, medical professionals frequently classify it as CIS. Multiple sclerosis does not always develop in CIS patients.
- Relapsing-remitting MS (RRMS): It is the most prevalent type. Relapses or exacerbations, which are other terms for flare-ups of new or worsened symptoms, are common in people with RRMS. Following are times of remission (when symptoms stabilise or go away).
- Primary progressive MS (PPMS): People with PPMS experience symptoms that slowly deteriorate over time without experiencing any relapses or remissions.
- Secondary progressive MS (SPMS): People with RRMS who subsequently develop SPMS are commonly diagnosed with SPMS. Multiple sclerosis that is secondary-progressive causes ongoing nerve damage. Your symptoms get worse with time. You no longer have periods of remission following relapses or flares (when symptoms worsen), even if you may still have some of these (when symptoms stabilise or go away).
Causes of Multiple Sclerosis
Experts are still unsure about the precise cause of multiple sclerosis. To assist pinpoint the disease’s underlying causes, research is ongoing. Several things can cause MS, such as:
Exposure to specific viruses or bacteria: According to some studies, MS may develop later in life if a person is exposed to particular illnesses (such as the Epstein-Barr virus).
Your residence: Your chance of acquiring MS may be influenced by your environment. The prevalence of the disease is noticeably higher in some regions of the world than others. MS is more prevalent in regions that are farthest from the equator. That might be because the sun doesn’t shine as brightly in certain areas. A risk factor for MS development is reduced vitamin D levels in people who spend less time in the sun.
Multiple sclerosis is an autoimmune disease, which affects the way your immune system works. Researchers are trying to determine why immune cells in some people attack healthy cells inadvertently.
Gene mutations: Having an MS-afflicted family member does enhance your likelihood of developing the condition. However, it is still unknown precisely how and which genes contribute to the onset of multiple sclerosis.
Early signs and symptoms
MS symptoms can appear in any part of the body since the CNS, which regulates all bodily processes, is affected by the disease.
The most typical signs of MS include:
Weak muscles:
People may experience weak muscles as a result of inactivity or stimulation brought on by nerve injury.
One of the first signs of MS is Numbness and tingling, which can affect the face, body, arms, and legs and feel like pins and needles.
Lhermitte’s sign:
When a person moves their neck, they could feel an electric shock-like sensation; this is referred to as Lhermitte’s sign.
Bladder issues:
Urge incontinence, or the sudden or frequent need to urinate, can make it difficult for a person to empty their bladder. An early indication of MS is losing control of one’s bladder.
Bowel issues:
Fecal impaction brought on by constipation might result in bowel incontinence.
One of the most typical symptoms of MS is fatigue, which can make it difficult for a person to perform at work or at home.
Along with balance and coordination impairments, vertigo and dizziness are frequent ailments.
Sexual dysfunction:
Both sexes may become uninterested in having sex.
Muscle spasms and stiffness:
are early signs of MS. Painful muscle spasms, particularly those in the legs, can be brought on by damage to the nerve fibres in the spinal cord and brain.
Tremor:
Some MS patients may have uncontrollable trembling.
Having trouble seeing:
Some people may have double, blurry, or even complete loss of eyesight. One eye is typically affected at a time by this. When the eye moves, pain due to optic nerve inflammation may be experienced. Vision issues are a precursor to MS.
Changes in gait and mobility:
MS can alter a person’s gait owing to muscle weakness, issues with balance, weariness, and dizziness.
Depression and emotional changes:
Demyelination and brain nerve fibre loss can cause emotional alterations.
Memory and learning issues:
These can make it difficult to focus, prioritise, learn, plan, and multitask.
Pain:
MS patients frequently experience pain. While localised pain may be brought on by muscle stiffness or spasticity, neuropathic pain is directly related to MS.
Less frequent signs include:
- headaches
- loss of hearing
- itching
- breathing or respiratory issues
- seizures
- speaking issues
- swallowing difficulties
Additionally, there is a greater chance of losing mobility, diminished activity, and urinary tract infections. A person’s career and social life may be impacted by these.
Risk factors for MS
There is still no known cause for MS. There are, however, a number of risk factors for MS development.
These risk elements consist of:
- having a family member with MS
- obesity
- some infections
- smoking
- a few autoimmune diseases, including type 1 diabetes and rheumatoid arthritis
How is multiple sclerosis (MS) managed or treated?
MS presently has no known cure. The main goals of treatment are to control symptoms, lessen relapses (times when symptoms return), and reduce the disease’s course. Your detailed treatment programme can include:
- Disease-modifying treatments (DMTs): The FDA has approved a number of drugs for the long-term treatment of multiple sclerosis (MS). These medications lessen relapses (also called flare-ups or attacks). They impede the spread of the illness. Additionally, they can stop the growth of new lesions on the spinal cord and brain.
- Relapse prevention drugs: Your neurologist could advise a high dosage of corticosteroids if you experience a severe attack. The drug has a rapid anti-inflammatory effect. They mitigate harm to your nerve cells’ protective myelin coating.
- Physical therapy: Multiple sclerosis might impair your physical capabilities. Maintaining your physical fitness and strength will assist your mobility.
- Counseling for mental health: Managing a chronic illness can be emotionally taxing. Furthermore, MS might occasionally impair your mood and memory. A crucial component of treating the condition is working with a neuropsychologist or receiving other emotional assistance.
REFREENCES:
- https://www.healthline.com/health/multiple-sclerosis
- https://www.medicalnewstoday.com/articles/37556
- https://my.clevelandclinic.org/health/diseases/17248-multiple-sclerosis
- https://www.webmd.com/multiple-sclerosis/guide/what-is-multiple-sclerosis
- https://www.mayoclinic.org/diseases-conditions/multiple-sclerosis/symptoms-causes/syc-20350269
For more details, kindly visit below.