Can Obstructive sleep apnea cause cognitive decline?
According to a study, people who have obstructive sleep apnea may experience cognitive decline.
The study is distinctive because all of its subjects were in good health and were free of the comorbid conditions that are frequently cited as the processes behind the association between sleep apnea and cognition.
According to the study, males as young as middle age can experience cognitive decline brought on by obstructive sleep apnea.
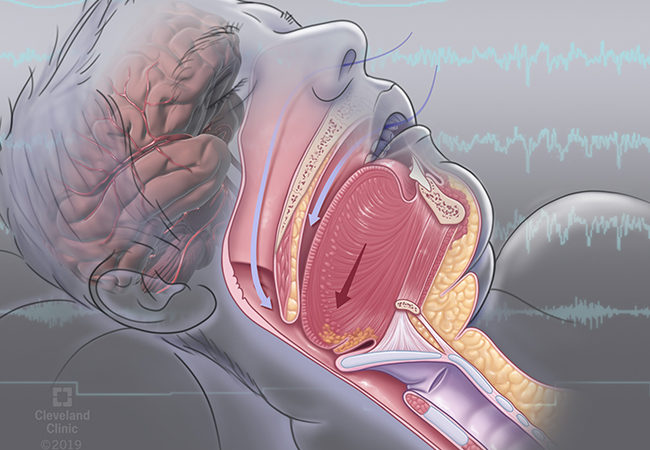
When a person has obstructive sleep apnea (OSA), their airway occasionally becomes obstructed for at least 10 seconds while they are asleep. It has been hypothesised that the cardiovascular or metabolic comorbidities that cause these breathing disruptions are the cause of the eventual decline in cognitive function.
According to a recent research of individuals without these comorbidities, sleep apnea itself can cause cognitive deterioration as early as age 40.
Men from a distinctive group took part in the study. People with systemic hypertension, hyperlipidemia, diabetes, cardiovascular disease, and other metabolic illnesses are more likely to be diagnosed with OSA.
This study is the first to examine the cognitive impact of OSA in otherwise healthy and non-obese persons because none of the study participants had any such comorbidities.
In their otherwise healthy subjects, the researchers discovered that OSA was associated with worsened executive function, visuospatial memory, vigilance (sustained attention), psychomotor function, and impulsive control.
Obstructive sleep apnea
According to a recent examination of data from 16 countries, 425 million adult men and women between the ages of 30 and 69 have moderate-to-severe OSA, and 936 million have mild-to-severe OSA. One estimate places the number of Americans with the illness at 25 million.
Sleep apnea might be one of two forms. The brain is unable to regularly signal the breathing muscles in people with less common central sleep apnea. OSA is more prevalent.
The dilator muscles that normally maintain the soft palate at the back of the throat open during breathing malfunction in people with obstructive sleep apnea or enable the tongue to impede the airway. Respiration is halted until the affected individual gasps or snorts to reopen the airway and restore breathing, which frequently happens before they completely awaken.
The link between obstructive sleep apnea and cognitive decline
According to the study’s findings, males who had severe obstructive sleep apnea had deficiencies in:
- Vigilance
- executive ability
- Visual recognition memory in the short term
- esteem on a social and emotional level
These issues were present in the males with mild obstructive sleep apnea as well, though not to the same extent as the individuals with severe versions of the illness. In reality, they hardly ever outperformed the control group in a meaningful way.
Even though the majority of men with sleep apnea had medical comorbidities, the study’s participants had none, including cardiovascular disease, diabetes, chronic inflammation, or depression. The authors pointed out that earlier studies blamed concomitant illnesses rather than sleep apnea for cognitive deficiencies.
Ivana Rosenzweig, MD, Ph.D., FRCPsych, a sleep specialist and consultant neuropsychiatrist, and the study’s lead author, said in an email to Healthline that “in our small proof-of-concept cross-sectional study, we demonstrated cognitive deficits in male patients with obstructive sleep apnea, even without any comorbidities.” This is extremely relevant because the current prevailing theory holds that cognitive deficiencies in this age range may be caused by comorbidities connected to obstructive sleep apnea.“
Rosenzweig stated, “Our research demonstrates that sleep apnea is sufficient to initiate cognitive alterations. Since the majority of these patients were (otherwise) healthy males with this condition, the vast majority of them were consciously ignorant that they already had cognitive abnormalities detected by the extremely sensitive testing battery.
The following are some potential causes of the cognitive issues, according to the researchers:
- sporadic low oxygen
- high blood carbon dioxide levels
- changes in the brain’s blood flow
- fragmented sleep
- Neuroinflammation
They stated that sleep apnea is a disorder that could be harmful.
Sleep apnea and dementia
The chance of developing dementia, including Alzheimer’s disease, may be considerably raised by sleep apnea. An assessment of research from 2022 found that it does not appear to raise the likelihood of acquiring vascular dementia.
Unfortunately, dementia can also cause sleep disruptions, according to Merrill. “Sleep disturbances increase dementia risk,” she said. As a result, your memory may eventually deteriorate to the point of dementia, which will make it harder for you to sleep. In this way, disturbed sleep can contribute to a downward spiral, making it even more crucial to recognize and address sleep problems during early and midlife adult development. Dementia affects sleep in several different ways, Merrill continued. “Dementia is a neurodegenerative illness, which means that brain cells begin to malfunction and die as time passes.
The brain’s sleep centres begin to malfunction when a person loses brain cells, making it harder for us to communicate with our bodies to stay asleep. Sleep is frequently broken up or even inverted, keeping patients awake all night before they fall asleep for the most of the day.
Merrill stated, “Ideally, sleep will be optimised years before the potential onset of dementia.” “With better sleep, we may be able to postpone the age at which dementia first manifests itself. To increase a person’s healthy life span as much as feasible, sleep quality should be improved.
The CDC recommends that those aged 61 to 64 receive seven to nine hours of sleep per night, while those aged 65 and over should aim for seven to eight hours.
Causes of OSA and cognitive damage
“Craniofacial and physiological particularities can be a risk factor for OSA — having a short chin, large tonsils, a large tongue, etc.,” said neuroscientist Dr. Nadia Gosselin from the University of Montreal in Canada, who was not involved in the study.
According to her, “these peculiarities increase a person’s risk of upper-airway obstruction during sleep.”
Although it is unclear how OSA causes cognitive loss, several of its fundamental characteristics, such as sleep disruption, intermittent hypoxemia, neuroinflammation, and oxidative stress, may be to blame.
According to Dr. Gosselin, OSA stops sleep from playing its part in memory consolidation, brain plasticity, and the elimination of cerebral metabolic waste by continuously fragmenting sleep.
She stated that systemic inflammation and blood-brain barrier disruption resulting in neuronal death are two more potential causes.
According to one study, the hippocampus and the entorhinal cortex, two areas of the brain that degrade quickly in Alzheimer’s disease, have higher levels of oxidative stress and inflammation.
How to treat sleep apnea
The good news is that OSA can frequently be treated by making small lifestyle adjustments, such eating better, working out more, and decreasing weight, she continued.
Through a range of therapy techniques, doctors can also assist patients in controlling OSA.
The CPAP machine, which uses continuous positive airway pressure to keep the airway open while you sleep, is the OSA technology that is used the most frequently. People with central sleep apnea may also be given medication, CPAP machines, or other breathing aids.
Other OSA therapies include oral mandibular advancement devices or dental appliances that prevent the tongue from obstructing the throat. Additionally, there are neurostimulation implants for OSA, and surgery can occasionally be beneficial.
REFERENCES:
- https://www.medicalnewstoday.com/articles/obstructive-sleep-apnea-and-cognitive-decline-study-suggests-direct-link
- https://www.healthline.com/health-news/sleep-apnea-may-increase-your-risk-of-cognitive-decline-dementia
- https://jamanetwork.com/journals/jamanetworkopen/fullarticle/2794441
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5281652/
For Cognitive decline medications that have been suggested by doctors worldwide are available here https://mygenericpharmacy.com/index.php?cPath=77_478