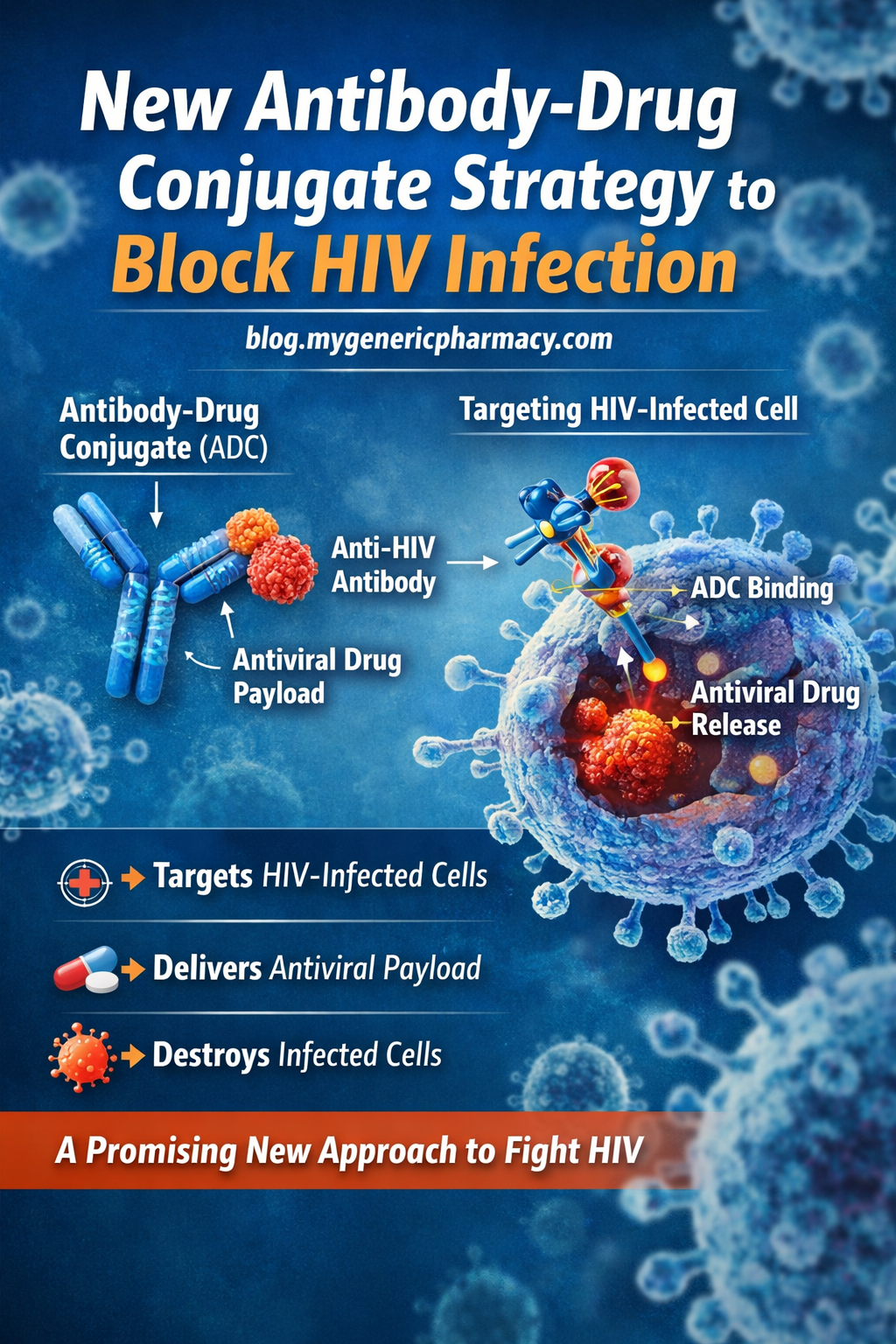
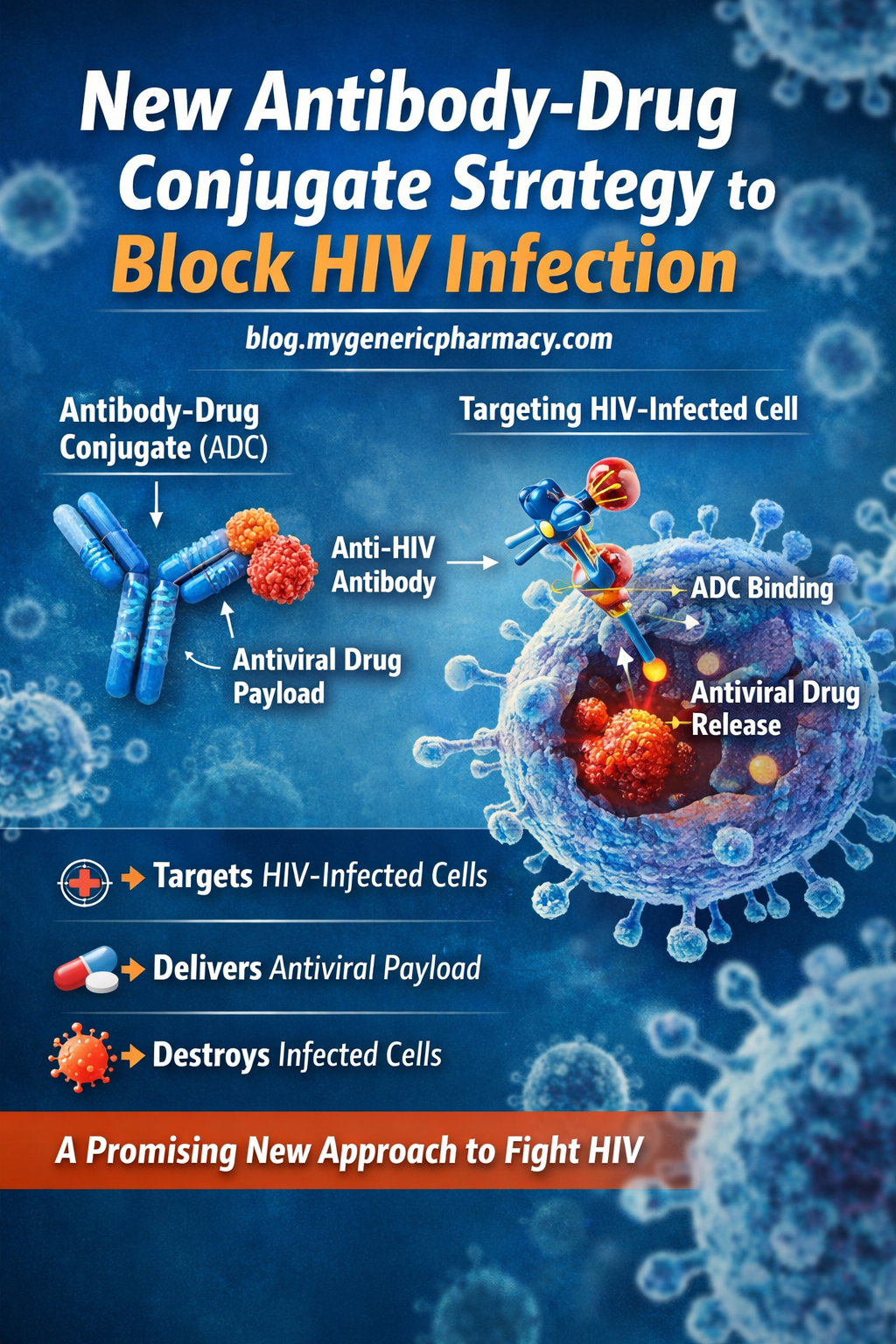
From Infection to Protection: The Complete Guide to Antiviral Medications
Viral infections—from seasonal flu to chronic diseases like hepatitis and HIV affect millions of people worldwide. Unlike bacterial infections, viruses require targeted treatment strategies. This is where antiviral medications play a critical role. In this comprehensive guide, we’ll explore how antiviral drugs work, their benefits, limitations, and what you need to know to use them safely.
What Are Antiviral Medications?
Antiviral medications are drugs designed to treat viral infections by inhibiting the development and spread of viruses within the body. Unlike antibiotics, which kill bacteria, antivirals work by interfering with the virus’s life cycle.
They are commonly used to treat:
- Influenza (flu)
- Herpes simplex virus
- Hepatitis B and C
- HIV
- COVID-19
How Do Antiviral Medications Work?
Viruses replicate by invading host cells and using them to produce more virus particles. Antiviral medications disrupt this process at different stages.
1. Blocking Viral Entry
Some antivirals prevent viruses from entering healthy cells, stopping infection early.
2. Inhibiting Replication
Many drugs interfere with viral genetic material, reducing the virus’s ability to multiply.
3. Preventing Viral Release
Certain antivirals stop new virus particles from leaving infected cells, limiting further spread.
This multi-targeted approach makes antivirals effective in controlling infections.
Common Antiviral Medications
Several antiviral drugs are widely used in clinical practice:
- Oseltamivir
- Acyclovir
- Remdesivir
- Tenofovir
Each medication is designed to target specific viruses and should be used under medical supervision.
Benefits of Antiviral Medications
1. Faster Recovery
Antivirals can shorten the duration of illness and reduce symptom severity when taken early.
2. Reduced Risk of Complications
They help prevent severe outcomes, especially in high-risk individuals such as the elderly or those with chronic conditions.
3. Lower Transmission
By reducing viral load, antivirals may decrease the risk of spreading infections to others.
4. Long-Term Disease Management
For chronic viral infections like HIV, antivirals allow patients to live longer, healthier lives.
When Should You Take Antivirals?
Timing is crucial. For conditions like influenza, medications such as Oseltamivir are most effective when started within 24–48 hours of symptom onset.
Doctors may also prescribe antivirals:
- For severe infections
- For immunocompromised patients
- As preventive therapy for certain exposures
Safety and Side Effects
Antiviral medications are generally safe but may cause side effects such as:
- Nausea
- Headache
- Fatigue
- Digestive discomfort
Serious side effects are rare but possible. Always follow your doctor’s guidance and avoid self-medication.
Limitations of Antiviral Drugs
Despite their benefits, antivirals have some limitations:
- They may not completely eliminate the virus
- Drug resistance can develop over time
- Not all viruses have effective antiviral treatments
- Effectiveness often depends on early use
Ongoing research continues to improve antiviral therapies and expand treatment options.
Supporting Your Immune System
In addition to medication, lifestyle choices can strengthen your body’s ability to fight infections:
- Eat a balanced diet rich in nutrients
- Stay hydrated
- Get adequate sleep
- Practice good hygiene
- Manage stress effectively
A strong immune system enhances the effectiveness of antiviral treatment.
Final Thoughts
Antiviral medications are a cornerstone of modern medicine, offering effective treatment and prevention for a wide range of viral infections. From acute illnesses like the flu to chronic conditions such as HIV, these drugs play a vital role in improving patient outcomes.
Medications like Acyclovir and Tenofovir have revolutionized care, making viral diseases more manageable than ever before.
Understanding how antivirals work—and using them responsibly—can help you protect your health and recover faster.
References:
- World Health Organization – Guidelines on viral infections and treatment
- Centers for Disease Control and Prevention – Antiviral medication usage and influenza treatment
- National Institutes of Health – Research on antiviral drug mechanisms
- U.S. Food and Drug Administration – Approval and safety of antiviral drugs
- Mayo Clinic – Clinical information on viral infections and treatments
Medications that have been suggested by doctors worldwide are available on the link below
https://mygenericpharmacy.com/category/anti-viral/famvir