Helpful things you must know about Coronary Artery Disease.
When the coronary arteries grow too thin or cholesterol blockages form in the walls), also known as coronary heart disease(CAD). The blood channels that carry blood and oxygen to the heart are known as the coronary arteries.
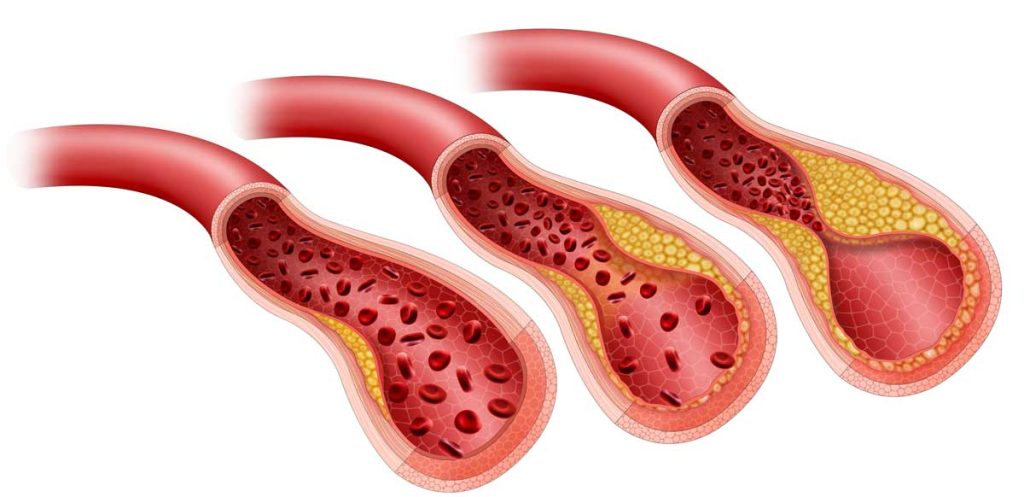
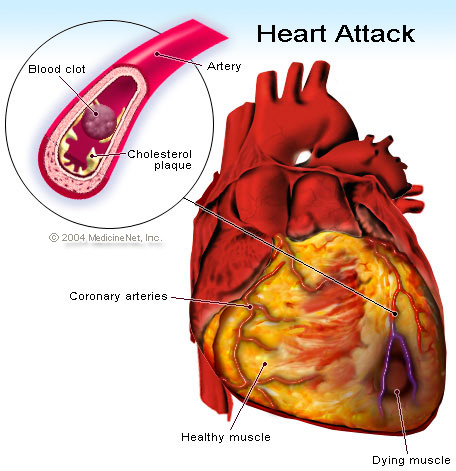
When cholesterol deposits on the arterial walls form plaques, CAD frequently results. These plaques can either produce inflammation and hardening of the blood vessel walls, which reduces blood flow to the heart and causes the arteries to constrict. Sometimes clots can impede blood flow, leading to major medical issues.
The network of blood vessels that supplies the surface of the heart with oxygen is made up of coronary arteries. The heart may not get enough oxygen-rich blood if these arteries are small, especially during exercising.
Forms of coronary artery disease
A heart attack can sometimes result from CAD. It is the most prevalent kind of heart disease in the United States, where it causes more than 655,000 fatalities annually, according to the Centers for Disease Control and Prevention.
Coronary artery disease primarily comes in two different forms:
Stable Ischemic heart disease
The chronic form is this. Your coronary arteries gradually tighten over a long period of time. Your heart receives less blood that is rich in oxygen with time. Even if you may experience certain symptoms, you can manage the illness on a daily basis.
Acute coronary syndrome
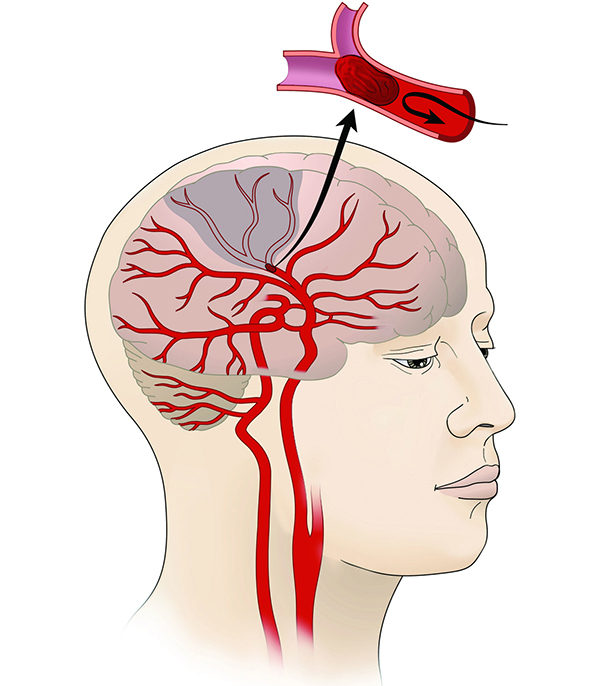
This is a medical emergency in its abrupt form. A blood clot is created when the plaque in your coronary artery abruptly bursts, obstructing blood flow to your heart. A heart attack is caused by this sudden obstruction.
How common is coronary artery disease?
Coronary artery disease affects a lot of people. In the US, there are about 18 million persons who have coronary artery disease. That almost equals the population of Houston, Chicago, Los Angeles, and New York City all together.
In the United States, coronary artery disease claimed 360,900 lives in 2019. That number of individuals could more than seven times fill Yankee Stadium.
What Causes CAD?
Plaque, which is made up of cholesterol, fat, and other chemicals, can begin to form on the blood vessel walls as early as childhood. It accumulates over time. This results in “atherosclerosis,” which doctors refer to as the hardening and narrowing of arteries.
Plaque may rupture or shatter in some circumstances. As a result, platelets, which are blood cells, will attempt to close the artery and create a blood clot.
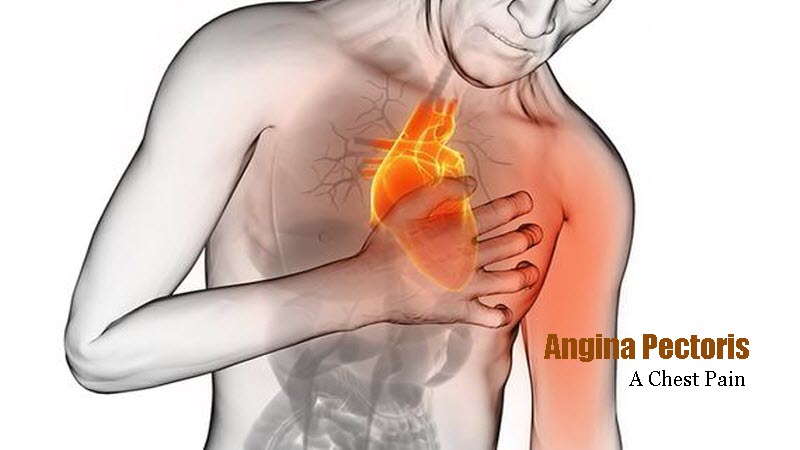
This accumulation hinders the free passage of blood through the arteries, much like muck in a clogged drainpipe. The heart receives nourishment and oxygen through the blood. It might cause chest pain and shortness of breath if you don’t get enough (Angina).
The heart can weaken if it doesn’t get enough oxygen. An erratic heartbeat may result from this (arrhythmia). It may also result in heart failure, which is the inability of the heart to adequately pump blood throughout the body to satisfy needs.
You may experience a heart attack if a plaque enlarges to the point where it obstructs blood flow to the heart muscle. However, the smaller plaques that rupture are typically the cause of heart attacks.
Coronary artery disease symptoms
Early on, you might not exhibit any signs. However, when the plaque keeps accumulating and restricts blood flow to the heart muscle, you could start to feel out of breath or exhausted, especially when you exercise.
Chest pain, often known as angina, is the most typical sign of CAD. Some individuals mistake it for indigestion or heartburn. Your chest may feel uncomfortable if you have angina. The feeling could also be felt in your back, shoulders, arms, or jaw.
You could feel:
- Tightness
- Discomfort
- Pressure
- Heaviness
- Squeezing
- Burning
- Aching
- Numbness
- Fullness
Call for emergency medical help if you experience any of the symptoms listed below.
- chest pain, especially in the centre or left side, that lasts for a short while or that disappears then reappears. It may feel like discomfort, squeezing, pressure, or fullness. Some individuals mistake it for heartburn or indigestion.
- Any discomfort in your upper torso. One or both arms, the shoulders, the neck, the jaw, or the upper section of the stomach could be affected.
- breathlessness with or without discomfort in the chest
- nausea or vomiting coupled with feeling faint, woozy, or cold
What puts you at Risk?
As you age or if it runs in your family, you are more prone to develop coronary artery disease (CAD). However, you may control a variety of additional risk factors, such as:
- High triglyceride and cholesterol levels
- elevated blood pressure
- Smoking
- Diabetes syndrome
- Overweight and obesity
- inadequate exercise
- Anger, sadness, and stress
- unsound diet
- excess booze
- Slumber apnea
Prevention
Keeping blood cholesterol levels under control can lower a person’s risk of developing CAD. Think about the following to improve blood cholesterol levels:
- being more active physically
- reducing alcohol consumption
- eschewing tobacco
- consuming a diet lower in salt, sugar, and saturated fats
Those who already have CAD should make careful to keep these factors under control by according to their doctor’s advice.
REFERENCES:
- https://www.healthline.com/health/coronary-artery-spasm
- https://www.medicalnewstoday.com/articles/184130
- https://my.clevelandclinic.org/health/diseases/16898-coronary-artery-disease
- https://www.webmd.com/heart-disease/coronary-artery-disease
- https://www.mayoclinic.org/diseases-conditions/coronary-artery-disease/symptoms-causes/syc-20350613
For more details, kindly visit below.